> Περίληψη
Ο κτηνίατρος καλείται συχνά να αντιμετωπίσει παθήσεις των δοντιών των ζώων συντροφιάς και αναγκάζεται αρκετά συχνά, επίσης, να προτείνει την εξαγωγή τους. Η περιοδοντική νόσος και τα κατάγματα δοντιών αποτελούν τις πιο συνήθεις ενδείξεις εξαγωγής δοντιών, ενώ οι διαταραχές της αιμόστασης ή άλλες παθήσεις που μπορεί να θέσουν σε κίνδυνο τη ζωή του ζώου αποτελούν αντένδειξη για την εξαγωγή δοντιού. Πριν από την έναρξη της διαδικασίας εξαγωγής δοντιού απαιτείται ο κατάλληλος προεγχειρητικός έλεγχος και η εφαρμογή τοπικής αναισθησίας και αναλγησίας. Η εξαγωγή διευκολύνεται με τη χρήση των κατάλληλων εργαλείων και μηχανημάτων. Περιγράφονται δύο τεχνικές αφαίρεσης δοντιών, η κλειστή τεχνική και η ανοιχτή ή χειρουργική τεχνική. Οι τεχνικές αυτές εφαρμόζονται ανάλογα με τον τύπο του δοντιού και την ένδειξη εξαγωγής του. Οι συχνότερες επιπλοκές της εξαγωγής δοντιών είναι το κάταγμα της ρίζας και η παραμονή της στο φατνίο, η μετεξακτική αιμορραγία και ο τραυματισμός γειτονικών ανατομικών στοιχείων. Κατά τη μετεγχειρητική περίοδο επιβάλλεται η χορήγηση των κατάλληλων αναλγητικών ή/και αντιμικροβιακών φαρμάκων και η καθοδήγηση των ιδιοκτητών σχετικά με τη διατροφή του ζώου, τη στοματική υγιεινή και τη μετεγχειρητική αξιολόγηση και παρακολούθηση.
> Εισαγωγή
Οι ιδιοκτήτες των ζώων συντροφιάς δείχνουν όλο και μεγαλύτερο ενδιαφέρον για τη γνώση, την πρόληψη και την αντιμετώπιση των νοσημάτων και των παθολογικών καταστάσεων της στοματικής κοιλότητας. Συνεπώς, ο κτηνίατρος έρχεται συχνά αντιμέτωπος με οδοντιατρικά περιστατικά στην καθημερινή κλινική πράξη, η αντιμετώπιση των οποίων, αρκετές φορές, στηρίζεται στην εξα- γωγή αριθμού δοντιών.
Άλλωστε, η ανάληψη και η παρακολούθηση οδοντιατρικών περιστατικών, μετά από την απόκτηση επαρκούς εμπειρίας για την διαχείριση τους, αποτελεί μη αμελητέο ποσοστό εσόδων ενός ιατρείου ζώων συντροφιάς.
> Ανατομική υπόμνηση
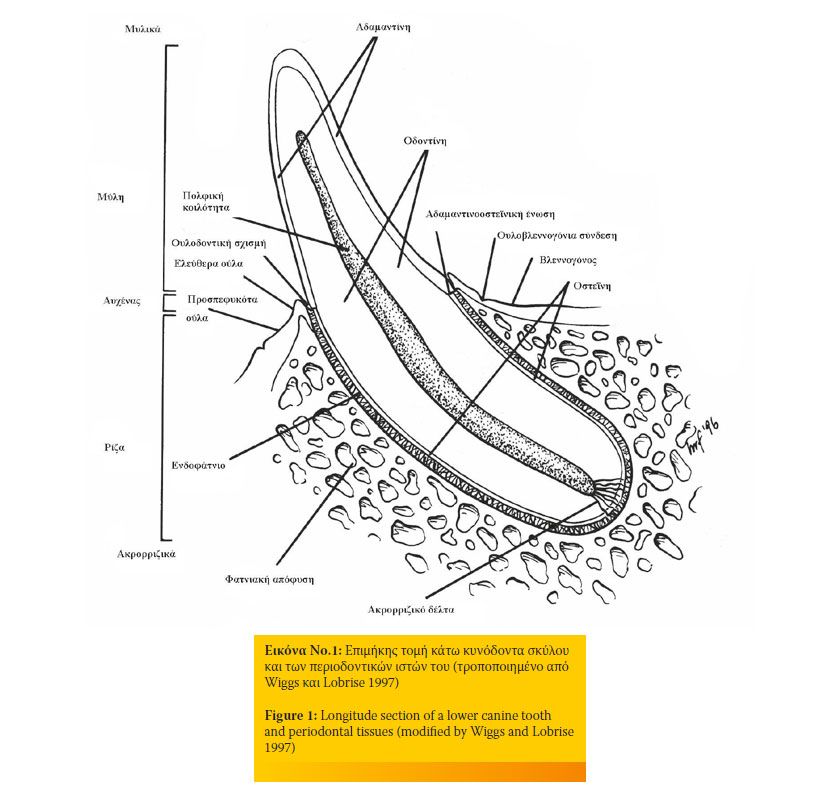
Στην Eικόνα 1 απεικονίζεται σε επιμήκη τομή ο κάτω κυνόδοντας του σκύλου. Σημειώνονται τα βασικά ανατομικά στοιχεία του δοντιού και των περιοδοντικών ιστών που το περιβάλλουν.
Τα δόντια του σκύλου, ο αριθμός των ριζών τους και ο αριθμός του κάθε δοντιού (ο πρώτος αριθμός αντιστοιχεί στο ημιμόριο της κάθε γνάθου και οι δύο επόμενοι στη θέση του δοντιού σε σχέση με τη μέση γραμμή, π.χ. ο μέσος άνω δεξιά τομέας αντιστοιχεί στον αριθμό 101) απεικονίζονται στην Eικόνα 2, ενώ στην Eικόνα 3 παρουσιάζονται τα δόντια της γάτας. Όπως φαίνεται και στις εικόνες υπάρχουν διαφορές στον αριθμό, στο μέγεθος και στο σχήμα των δοντιών μεταξύ των δύο ειδών. Λόγω του μεγέθους και του σχήματός τους τα δόντια της γάτας είναι αρκετά πιο εύθραυστα σε σχέση με εκείνα του σκύλου.
> Ενδείξεις εξαγωγής δοντιών
Η εξαγωγή των δοντιών αποτελεί μια από τις συνηθέστερες επεμβάσεις της χειρουργικής των ζώων συντροφιάς, την οποία καλείται να εκτελέσει συχνά ο κτηνίατρος κατά την άσκηση του επαγγέλματος. Οι ενδείξεις για την «απομάκρυνση» ενός ή περισσότερων δοντιών παρατίθενται αμέσως παρακάτω:
1. Δόντια τα οποία πάσχουν από περιοδοντική νόσο: αποτελούν την πιο συχνή ένδειξη εξαγωγής δοντιού στο σκύλο και στη γάτα. Εξαγωγή στα δόντια αυτά πραγματοποιείται όταν:
α) υπάρχει εκτεταμένη καταστροφή των περιοδοντικών ιστών, μεγαλύτερη από το 50%, του μήκους της ρίζας. Η απώλεια πρόσφυσης των στηρικτικών ιστών του δοντιού χαρακτηρίζεται από εκβάθυνση της ουλοδοντικής σχισμής (θύλακας) ή/και από υποχώρηση των ούλων (υφίζηση)
β) η κινητικότητα (ευσειστότητα) είναι μεγαλύτερη από 1 mm
γ) έχει προκληθεί δευτερογενώς ενδοδοντική νόσος
δ) έχει προκληθεί στοματορινικό συρίγγιο
ε) υπάρχει αποκάλυψη του μεσορριζικού χώρου σε πολύρριζα δόντια.1,2
2. Τερηδόνα: η εξαγωγή των τερηδονισμένων δοντιών αφορά κυρίως στο σκύλο, σε περιπτώσεις που το μεγαλύτερο τμήμα της μύλης είναι κατεστραμμένο ή έχει προσβληθεί ο πολφός.2 Συχνότερα εξάγονται ο 1ος και ο 2ος γομφίος τόσο της άνω όσο και της κάτω γνάθου. Όταν η καταστροφή των δοντιών δεν είναι εκτεταμένη η εξαγωγή επιλέγεται, μόνο, εφόσον η αποκατάσταση ή η ενδοδοντική θεραπεία δεν είναι εφικτές.3
3. Απορρόφηση οδοντικής ουσίας (κυρίως στη γάτα): όταν οι απορροφήσεις είναι 2ου 3ου ή 4ου σταδίου1 και το δόντι είναι μη βιώσιμο και προκαλεί πόνο.4
4. Χρόνια ουλοστοματίτιδα της γάτας ή στοματίτιδα λόγω ανοσοανεπάρκειας: Η μικροβιακή πλάκα των δοντιών και ειδικότερα τα αναερόβια Gram αρνητικά βακτήρια φαίνεται πως εμπλέκονται στην παθογένεια και στην εξέλιξη της νόσου, οπότε η εξαγωγή ορισμένων ή και όλων των δοντιών είναι επιβεβλημένη.5,6
5. Κατάγματα των δοντιών: απόλυτη ένδειξη εξαγωγής αποτελούν τα λοξά κατάγματα που αφορούν τόσο στη μύλη όσο και στη ρίζα του δοντιού.7 Τα κατάγματα των δοντιών στα οποία αποκαλύπτεται ο πολφός θα πρέπει να αντιμετωπιστούν είτε με ενδοδοντική θεραπεία είτε να εξαχθούν.2
6. Δόντι ή δόντια που βρίσκονται στη γραμμή κατάγματος της άνω ή κάτω γνάθου: θα πρέπει να εξάγονται μόνο όταν εμφανίζουν προχωρημένη ή βαριά περιοδοντική νόσο,3 εάν είναι ιδιαίτερα εύσειστα ή εάν έχουν υποστεί βαρύ κάταγμα μύλης και ρίζας.5
7. Παραμένοντα νεογιλά δόντια: νεογιλά δόντια που δεν αποπίπτουν μετά τον 7ο μήνα της ηλικίας (συνηθέστερα οι νεογιλοί κυνόδοντες) εμποδίζουν την εξέλιξη της μόνιμης οδοντοφυΐας, δημιουργούν ορθοδοντικές ανωμαλίες και προδιαθέτουν σε περιοδοντική νόσο των μόνιμων δοντιών και θα πρέπει να εξάγονται το συντομότερο δυνατόν.3,7
8. Έγκλειστα, ημιέγκλειστα και μη λειτουργικά δυσπλαστικά δόντια: τα έγκλειστα δόντια είναι εκείνα που δεν ανατέλλουν και καλύπτονται από μαλακούς ιστούς ή/και από οστό. Τα ημιέγκλειστα δόντια έχουν αποτύχει να ανατείλουν πλήρως στην κανονική τους θέση. Τα έγκλειστα και τα ημιέγκλειστα δόντια θα πρέπει να εξάγονται εάν δημιουργούν προβλήματα, αλλιώς παρακολουθούνται, ώστε να προληφθεί μόλυνση, νέκρωση, δημιουργία οδοντογενών κύστεων ή νεοπλασματική εξαλλαγή των κύστεων.3
9. Υπεράριθμα δόντια: πρέπει να εξάγονται διότι οδηγούν σε ταχύτερη εμφάνιση και εξέλιξη της περιοδοντικής νόσου και σε ορθοδοντικά προβλήματα.3,6,7,8
10. Σε μη φυσιολογική σύγκλειση, τα δόντια τα οποία τραυματίζουν τους μαλακούς ιστούς θα πρέπει να εξάγονται, ειδικά εάν έχουν αποτύχει άλλες τεχνικές αντιμετώπισης του προβλήματος.6,8
11. Σε περιπτώσεις περιακρορριζικής φλεγμονής που μπορεί να οφείλεται σε ενδοδοντική ή σε περιοδοντική νόσο. Ακόμη, είναι απαραίτητο να εξάγονται δόντια τα οποία είναι υπαίτια για δημιουργία αποστήματος ή και πρόκλησης νέκρωσης του οστού και οστεομυελίτιδας.3
12. Δόντια τα οποία βρίσκονται εντός των ορίων νεοπλασμάτων της στοματικής κοιλότητας ή οδοντογενών κύστεων πρέπει να απομακρύνονται.3,8
13. Οικονομικοί και υποκειμενικοί παράγοντες που ωθούν τους ιδιοκτήτες να επιλέξουν την εξαγωγή από άλλες εναλλακτικές θεραπείες.3,8,9,10,11
> Αντενδείξεις
Όπως σε κάθε χειρουργική επέμβαση έτσι και στην εξαγωγή του δοντιού υπάρχουν περιπτώσεις που λόγω άλλων προβλημάτων υγείας του ζώου δεν μπορεί να πραγματοποιηθεί η χειρουργική διαδικασία.
Η εξαγωγή δοντιού αντενδείκνυται, χωρίς να προηγηθεί η κατάλληλη θεραπεία, σε ζώα με σοβαρές αιματολογικές διαταραχές,3,7,9 όπως για παράδειγμα σε διαταραχή των παραγόντων πήξης ή σε θρομβοκυτταροπενία. Επίσης, δεν προτείνεται σε ζώα που πάσχουν από βαριά νοσήματα όπως η λευχαιμία ή παρουσιάζουν υπέρταση, καθώς καθυστερεί η επούλωση του χειρουργικού τραύματος. Υπό προϋποθέσεις αντενδείκνυται, σε ζώα που λαμβάνουν αντιπηκτικά φάρμακα, ορισμένα μη στεροειδή αντιφλεγμονώδη (π.χ. Ασπιρίνη), αντινεοπλασματικά φάρμακα ή γενικότερα οποιαδήποτε αγωγή η οποία μπορεί προκαλέσει παρατεταμένη αιμορραγία.3,9 Ακόμη, είναι αυτονόητο ότι η εξαγωγή αποφεύγεται σε ζώα τα οποία λόγω συστηματικών νοσημάτων δεν μπορούν να υποβληθούν σε γενική αναισθησία,3,9 όπως σε τελικού σταδίου ηπατική και νεφρική ανεπάρκεια, βαριά υπέρταση, καρδιακές αρρυθμίες, βαριά νοσήματα του αναπνευστικού συστήματος κ.α. Ακόμη, δεν πρέπει να πραγματοποιείται, σε ζώα στα οποία εφαρμόζεται ακτινοθεραπεία στις γνάθους.3,9 Τέλος, σε κακοήθη νεοπλάσματα ή αιμαγγειώματα των γνάθων, η εξαγωγή του δοντιού μπορεί να επηρεάσει αρνητικά την πρόγνωση.9
> Διαδικασία εξαγωγών
Προεγχειρητικός Έλεγχος
Προεγχειρητικά, θα πρέπει να εκτιμηθεί η συνολική κλινική εικόνα της στοματικής κοιλότητας, αλλά και η κατάσταση του κάθε δοντιού, ως προς την κατάσταση του περιοδοντίου, την κινητικότητά του και την κατάσταση της μύλης του (εκτεταμένη απορρόφηση της μύλης μπορεί να έχει ως αποτέλεσμα το κάταγμα του δοντιού κατά την προσπάθεια εξαγωγής του).12
Τα προεγχειρητικά ακτινογραφήματα (προτιμότερο ενδοστοματικά) είναι απαραίτητα για την αξιολόγηση της μορφολογίας του δοντιού και την έκταση της παθολογικής κατάστασης που καθιστά αναγκαία την εξαγωγή.7 Είναι σημαντικό να καθοριστεί η διαμόρφωση των ριζών, η εγγύτητα σε παρακείμενα δόντια και άλλες σημαντικές δομές, καθώς και η κατάσταση του περιβάλλοντος οστού.12,13 Ακόμη, με την ακτινογράφηση εκτιμάται η κατάσταση του φατνιακού οστού, διαφο- ροποιήσεις σε σχέση με την φυσιολογική ανατομία των ριζών και η παρουσία οδοντοφατνιακής αγκύλωσης ή απορρόφησης των ριζών που θα μπορούσαν πιθανώς να επιπλέξουν την διαδικασία εξαγωγής.3,13 Τέλος, τα ακτινογραφήματα παρέχουν τεκμήρια για το ιατρικό αρχείο και μπορούν να χρησιμοποιηθούν ως μέσο “πειθούς” για τη συγκατάθεση του ιδιοκτήτη στην παροχή της απαιτούμενης φροντίδας.15
Σε ζώα με προϋπάρχουσες παθολογικές καταστάσεις απαιτούνται ιδιαίτερες προφυλάξεις, ώστε α αποτραπεί η μόλυνση, να ελαχιστοποιηθεί η αιμοραγία και να αποφευχθεί η επιδείνωση της νοσολογικής κατάστασής τους.14 Επίσης, όπως προαναφέρθηκε, για την εξαγωγή των δοντιών απαιτείται γενική αναισθησία, συνεπώς επιβάλλεται ο προεγχειρητικός αιματολογικός και βιοχημικός έλεγχος, ο οποίος θα εξασφαλίσει ότι το ζώο θα υποβληθεί σε γενική αναισθησία με ασφάλεια. Ασθενή ζώα με μη ελεγχόμενα μεταβολικά νοσήματα (π.χ. μη ελεγχόμενος σακχαρώδης διαβήτης, βαριά νεφρική ανεπάρκεια, μη αντισταθμιζόμενη καρδιακή νόσος ή μη διαχειρίσιμη διαταραχή της πήξης) δεν μπορούν να υποβληθούν σε γενική αναισθησία και εκτεταμένη επέμβαση στην στοματική κοιλότητα. Ενώ η διαχείριση της στοματικής ασθένειας μπορεί να βελτιώσει την ποιότητα ζωής του ζώου, το χειρουργείο θα πρέπει να αναβάλλεται μέχρι να τεθεί υπό έλεγχο το νόσημα.15,16
Αναλγησία, Γενική και Τοπική Αναισθησία
Η προληπτική διαχείριση του πόνου συμβάλλει στην ομαλή πορεία της γενικής αναισθησίας, σε καλή ανάνηψη και σε μειωμένο μετεγχειρητικό πόνο. Η χρήση αναλγητικών φαρμάκων με διαφορετικό τρόπο δράσης συντελεί στην μείωση του επώδυνου ερεθίσματος. Χρησιμοποιούνται κυρίως τέσσερις κατηγορίες φαρμακευτικών ουσιών: οπιοειδή, μη στεροειδή αντιφλεγμονώδη, α2 αγωνιστές και τοπικά αναισθητικά.16,17,18,19,20,21
Ειδικά η χορήγηση τοπικών αναισθητικών μειώνει την ανάγκη αύξησης του αναισθητικού βάθους, μειώνοντας τους κινδύνους της γενικής αναισθησίας και επιτρέποντας ταχύτερη ανάνηψη. Κυρίως χρησιμοποιούνται η λιδοκαΐνη και η μπουπιβακαΐνη σε οδοντιατρικά σκευάσματα που μπορεί να περιέχουν ή όχι επινεφρίνη (αγγειοσυσταλτικό). Οι κυριότερες επιπλοκές που μπορεί να προκύψουν από την χορήγηση τοπικής αναιθησίας είναι ο τραυματισμός κάποιου νεύρου, η πρόκληση αιματώματος και η ενδοαγγειακή έγχυση του αναισθητικού Η χρήση βελόνας μικρής διαμέτρου και η πραγματοποίηση αναρρόφησης πριν την έγχυση του αναισθητικού προλαμβάνουν σε ικανοποιητικό βαθμό τις επιπλοκές αυτές.16,17,18,19,20,21,22,23
Ανάλογα με το σημείο της στοματικής κοιλότητας στο οποίο θα επέμβουμε, έχουμε την δυνατότητα εφαρμογής στελεχιαίας τοπικής αναισθησίας ή τοπικής διήθησης των ιστών, με τα κυριότερα σημεία εφαρμογής που αναφέρονται να είναι τα εξής: 5,16,17,18,19,20,21,22,23
- Γενειακό νεύρο, το οποίο εξέρχεται από το γενειακό τρήμα. Με αυτό τον τρόπο αναισθητοποιούνται οι σύστοιχοι τομείς, οι κυνόδοντες και οι πρώτοι 1-2 προγόμφιοι της κάτω γνάθου (Εικόνα 4).
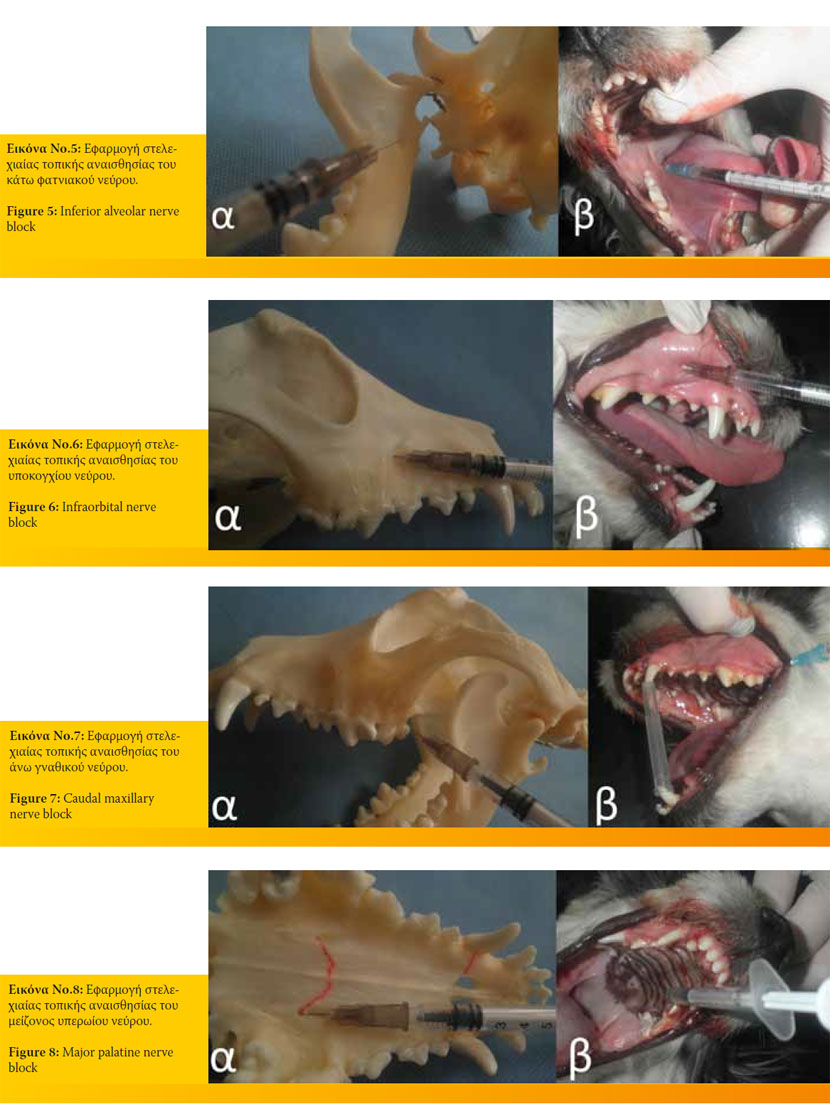
- Κάτω φατνιακό νεύρο, το οποίο εξέρχεται από το γναθιαίο τρήμα. Η προσέγγιση μπορεί να είναι ενδοστοματική ή εξωστοματική και επιτυγχάνεται αναισθητοποίηση όλων των σύστοιχων δοντιών του ημιμορίου της κάτω γνάθου (Εικόνα 5).
- Υποκόγχιο νεύρο, το οποίο εξέρχεται από το υποκόγχιο τρήμα. Επιτυγχάνεται η αναισθητοποίηση των σύστοιχων τομέων, των κυνοδόντων και των προγομφίων, ενώ υπό προυποθέσεις και εφαρμογή τροποποιημένης τεχνικής είναι εφικτή η αναισθητοποίηση και του 1ου γομφίου (Εικόνα 6).
- Άνω γναθικό νεύρο. Η προσέγγιση του μπορεί να είναι ενδοστοματική ή εξωστοματική και με αυτό τον τρόπο αναισθητοποιούνται όλα τα δόντια του σύστοιχου ημιμορίου της άνω γνάθου (Εικόνα 7).
- Μείζον υπερώιο νεύρο. Η προσέγγιση του είναι ενδοστοματική και επιτυγχάνεται με την είσοδο της βελόνας στο πρόσθιο στόμιο του υπερώιου πόρου. Με τη μέθοδο αυτή επιτυγχάνεται η αναισθητοποίηση του 4ου προγομφίου και των σύστοιχων δύο άνω γομφίων. Μπορεί να χρησιμοποιηθεί και επικουρικά εκείνης του υποκογχίου νεύρου (Εικόνα 8).
- Έγχυση τοπικού αναισθητικού υποπεριοστικά, ενδοφατνιακά, ενδοοστικά, ενδοπολφικά και εσωτερικά του μεσοδόντιου διαστήματος για κάθε δόντι ξεχωριστά.
Η διατήρηση της γενικής αναισθησίας με εισπνευστικά αναισθητικά είναι η πιο κοινή μέθοδος για χειρουργικές επεμβάσεις στη στοματική κοιλότητα. Στα πιο διαδεδομένα εισπνευστικά αναισθητικά περιλαμβάνονται τα: αλοθάνιο, ισοφλουράνιο, σεβοφλουράνιο και δεσοφλουράνιο16,21. Ακόμη και αν η γενική αναισθησία διατηρείται με ενέσιμο αναισθητικό φάρμακο, είναι απαραίτητη η χρήση ενδοτραχειακού σωλήνα με διατεταμένο αεροθάλαμο, για την αποφυγή εισρόφησης υγρών, οδοντικής τρυγίας, ιστικών υπολειμμάτων και μικροτεμαχίων.3,5,13,16,19,21,24,25 Επιπλέον προστασία παρέχει η τοποθέτηση σπληνίων γάζας ή σπόγγου στο φάρυγγα (μάλιστα προτείνεται η σύδεσή τους με ένα χρησιμοποιημένο ράμμα, το οποίο να εξέχει από τη στοματική κοιλότητα, ώστε να μην υπάρχει κίνδυνος παραμονής τους), το οποίο θα προσροφά και θα συγκρατεί τα παραπάνω αναφερόμενα υλικά. Χρήσιμη κρίνεται και η κατά διαστήματα αναρρόφηση με ανάλογη συσκευή, προς απομάκρυνση των υλικών αυτών. Επισημαίνεται ότι η αφαίρεση των γαζών ή του σπόγγου προηγείται αυτής του τραχειοσωλήνα.5,13,16,19,21,25 Σε κάθε περίπτωση είναι απαραίτητος ο καθετηριασμός κάποιας φλέβας, ώστε να υπάρχει άμεση πρόσβαση και δυνατότητα χορήγησης υγρών και φαρμακολογικής υποστήριξης (αντιμικροβιακών φαρμάκων, ινοτρόπων, αγγειοσυσπαστικών φαρμάκων) αν κριθεί απαραίτητο.16,21 Καθ’ όλη την διάρκεια της γενικής αναισθησίας θα πρέπει να δίνεται η απαιτούμενη σημασία στον έλεγχο των ζωτικών λειτουργιών του ασθενούς (καρδιακή λειτουργία, αναπνευστική λειτουργία, χροιά βλεννογόνων, θερμοκρασία ασθενούς κ.α.).16,20,21
Απαραίτητος Εξοπλισμός
Στον βασικό ειδικό οδοντιατρικό εξοπλισμό για την εκτέλεση επεμβάσεων εξαγωγής δοντιών περιλαμβάνονται:
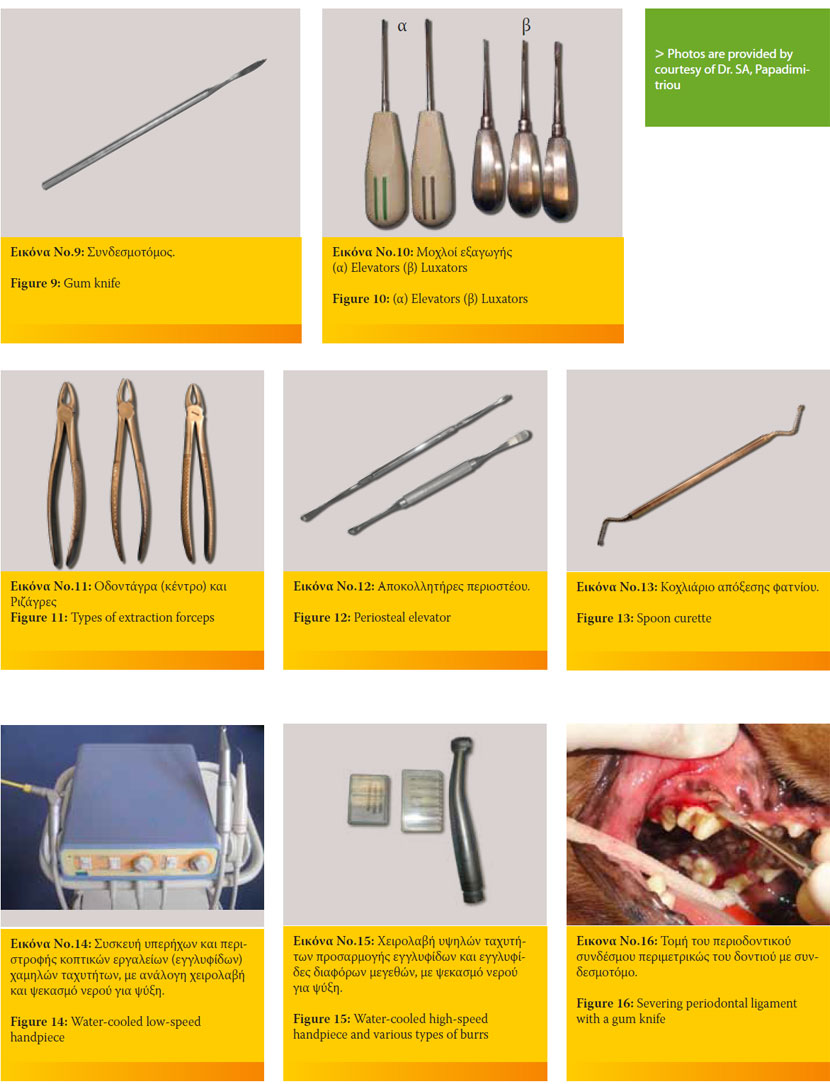
- ο συνδεσμοτόμος που βρίσκει εφαρμογή στην αρχική τομή των ινών του ενδοφατνίου ή περιοδοντικού συνδέσμου (Εικόνα 9).5
- οι μοχλοί εξαγωγής που διακρίνονται σε luxators (διεισδύουν στον περιορισμένο περιοδοντικό χώρο και τέμνουν τις ίνες του ενδοφατνίου), και σε elevators (εισάγονται με ήπιο τρόπο στον χώρο μεταξύ του δοντιού και του φατνιακού οστού, και ύστερα από ελεγχόμενη περιστροφική κίνηση, προκαλούν ρήξη του ενδοφατνίου). Η βασική διαφορά τους είναι ότι οι luxators φέρουν λεπτότερο και αιχμηρότερο άκρο από τους elevators και βρίσκουν εφαρμογή στην αρχή της διαδικασίας εξαγωγής, με τους elevators και τις οδοντάγρες να ακολουθούν, αν αυτό κριθεί απαραίτητο1,3,12,25,26,27 (Εικόνα 10).
- οι οδοντάγρες (που χρησιμοποιούνται για την απομάκρυνση εύσειστων δοντιών από το φατνίο) και οι ριζάγρες (οι οποίες βρίσκουν εφαρμογή στην απομάκρυνση υπολειπόμενων τμημάτων δοντιών ή ριζών καθώς και δοντιών μικρού μεγέθους) (Εικόνα 11).1,12,25,26,27,28
- o αποκολλητήρας περιοστέου που χρησιμοποιείται για την αποκόλλησή του κατά την διαδικασία παρασκευής βλεννογονοπεριοστικού κρημνού ολικού πάχους στην χειρουργική τεχνική εξαγωγής (Εικόνα 12).25,26,28
- το κοχλιάριο απόξεσης για τον καθαρισμό και τη λείανση του φατνίου μετά την εξαγωγή του δοντιού28 (Εικόνα 13).
- συσκευή περιστροφής κοπτικών εργαλείων χαμηλής (micromotor, συνήθως μέχρι 30- 35.000 στροφές/λεπτό) (Εικόνα 14) ή υψηλής ταχύτητας (300- 400.000 στροφές/λεπτό), με ψεκασμό νερού για ψύξη, που δέχονται την προσαρμογή εξαρτημάτων (εγγλυφίδων διαμαντιού ή καρβιδίου, δίσκου κοπής κ.α.) (Εικόνα 15) και χρησιμοποιούνται στην τομή των δοντιών και στην αφαίρεση του φατνιακού οστού.5,25,26
> Γενικές Αρχές και Τεχνικές Εξαγωγών
Γενικές αρχές χειρουργικής των εξαγωγών
Όπως σε κάθε χειρουργική επέμβαση, έτσι και στις εξαγωγές θα πρέπει να τηρούνται κάποιες γενικές αρχές. Είναι απαραίτητη η γνώση της ανατομίας της στοματικής κοιλότητας, των γνάθων και των δοντιών, ώστε να αποφεύγονται ιατρογενείς τραυματισμοί. Επίσης, απαιτείται καλή ορατότητα στην περιοχή, η οποία εξασφαλίζεται από μια καλή πηγή φωτός.7,13,25,29
Νερό ή συνδυασμός αέρα και νερού από μια αεροσύριγγα/υδροσύριγγα χρησιμοποιείται για την απομάκρυνση ιστικών μικροτεμαχίων και διαφόρων υπολειμμάτων, για την αφύγρανση της περιοχής χρησιμοποιείται μόνο αέρας,7 ενώ χρήσιμη είναι και μια συσκευής αναρρόφησης.13,19,29
Το ζώο τοποθετείται σε πλάγια ή σε ραχιαία κατάκλιση2,12 με τρόπο ώστε να διευκολύνεται ο χειρουργός.13,29,30 Επιπλέον, οι ήπιοι χειρισμοί αποτρέπουν τον τραυματισμό τόσο των μαλακών όσο και των σκληρών ιστών, ενώ συμβάλλουν στην γρηγορότερη επούλωσή τους.2,13
Λόγω των ιδιομορφιών του περιβάλλοντος της στοματικής κοιλότητας δεν είναι δυνατόν να πραγματοποιηθεί άσηπτη επέμβαση σε αυτή, ωστόσο ο περιορισμός των παθογόνων βακτηρίων στην περιοχή είναι σημαντικός. Η αποτρύγωση και η στίλβωση των δοντιών, ακολουθούμενη από προεγχειρητική έκπλυση με διάλυμα γλυκονικής χλωρεξιδίνης,3,12,29,31 συμβάλει στην μείωση της βακτηριαιμίας. Επίσης, αποτρέπει τη μόλυνση του μετεξακτικού φατνίου απο την τρυγία και άλλα ιστικά υπολείμματα, η οποία μπορεί να παρεμποδίσει τη φυσιολογική επούλωση του τραύματος.3 Η προεγχειρητική χορήγηση αντιμικροβιακών φαρμάκων ευρέως φάσματος ή με δράση κατά των αναεροβίων βακτηρίων (αμοξικιλλίνη-κλαβουλανικό κάλιο, κλινδαμυκίνη, μετρονιδαζόλη)31 ενδείκνυται σε ζώα που πάσχουν από ενδοκρινοπάθεια, καρδιαγγειακή νόσο και γενικότερα από σοβαρή τοπική ή συστηματική νόσο ή είναι εξασθενημένα και ανοσοκατασταλμένα, με σκοπό την έγκαιρη αντιμετώπιση της βακτηριαιμίας που αναπόφευκτα προκύπτει κατά τις οδοντιατρικές επεμβάσεις.3,24,31 Είναι σημαντικό τα φάρμακα αυτά να βρίσκονται σε ικανοποιητική συγκέντρωση στο πλάσμα του αίματος τη στιγμή της οδοντιατρικής επέμβασης, για αυτό και ενδείκνυται η ενδοφλέβια χορήγησή τους αμέσως μετά την αναισθητοποίηση του ζώου.18
Για την αποτροπή επαφής με αερολυμένα βακτήρια, μικροσταγονίδια και μικροτεμάχια ιστών, ο επεμβαίνων θα πρέπει να φορά μάσκα, γάντια, κατάλληλο ιματισμό και προστατευτικά οφθαλμών,12,20,25,29,30 ενώ επιβάλλεται ο καλός αερισμός του χώρου.25,29
Τεχνικές εξαγωγής δοντιών
Εξαγωγές δοντιών μπορούν να πραγματοποιηθούν είτε με την κλειστή τεχνική (χωρίς την παρασκευή βλεννογονοπεριοστικού κρημνού) είτε με την ανοικτή-χειρουργική τεχνική (παρασκευή και ανύψωση βλεννογονοπεριοστικού κρημνού ώστε να αποκαλυφθεί το φατνιακό οστό).3
Κατά την κλειστή τεχνική εφαρμόζονται δυνάμεις εκμόχλευσης και τελικά έλξης στα υπό εξαγωγή δόντια με τη χρήση των εργαλείων που προαναφέρθηκαν, χωρίς να είναι αναγκαία η αφαίρεση τμήματος φατνιακού οστού.7 Ενδείκνυται για την εξαγωγή δοντιών με σχετικά μικρό μήκος ρίζας, εύσειστων λόγω περιοδοντίτιδας ή τραυματισμού, αλλά και μονόριζων δοντιών (τομέων) ή προγομφίων μετά από διαχωρισμό τους.1,5
Στην ανοικτή τεχνική παρασκευάζεται και ανασηκώνεται ο βλεννογονοπεριοστικός κρημνός, ώστε να αποκαλυφθεί το φατνιακό οστό. Συνήθως αφαιρείται το τμήμα του φατνιακού οστού που καλύπτει την παρειακή επιφάνεια της ρίζας του δοντιού, ώστε να διευκολυνθεί η αφαίρεσή του. Ο βλεννογονοπεριοστικός κρημνός επανατοποθετείται στη φυσιολογική θέση του και συρράπτεται, ώστε να επουλωθεί κατα α’ σκοπό το μετεξακτικό φατνίο.7 Ενδείκνυται για την εξαγωγή δοντιών με μεγάλες ρίζες, όπως οι κυνόδοντες ή ο πρώτος γομφίος της κάτω γνάθου, πολύρριζα δόντια όπως ο 4ος προγόμφιος και ο 1ος γομφίος της άνω γνάθου και γενικότερα σε δόντια με ισχυρή πρόσφυση στο φατνίο ή σε πολλαπλές εξαγωγές στο ίδιο ημιμόριο μιας γνάθου.1,5
Η επιλογή της κλειστής ή της χειρουργικής τεχνικής βασίζεται σε αρκετούς παράγοντες. Οι πιο σημαντικοί είναι η μορφολογία του προς εξαγωγή δοντιού, η υπάρχουσα παθολογική κατάσταση και η προτίμηση του επεμβαίνοντος.7
Η βασική διαφοροποίηση (και στις δύο τεχνικές) όσον αφορά την εξαγωγή μονόριζου ή πολύρριζου δοντιού, είναι η τομή του πολύρριζου δοντιού με τη χρήση εγγλυφίδας σε χειρολαβή χαμηλών ή υψηλών ταχυτήτων σε ισάριθμα τμήματα με τον αριθμό των ριζών του. Στη συνέχεια τα τμήματα αυτά εξάγονται όπως και τα μονόριζα δόντια. Απαραίτητη προυποθέση για την επιτυχή ολοκλήρωση αυτού του σταδίου είναι ο προηγούμενος εντοπισμός του μεσορρίζιου διαστήματος.5
Κατά την κλειστή τεχνική ακολουθούνται τα εξής βήματα:
1. Αρχικά πραγματοποιείται τομή του περιοδοντικού συνδέσμου περιμετρικώς του δοντιού με συνδεσμοτόμο ή με νυστέρι Νο11 ή Νο15, το οποίο εισάγεται στην ουλοδοντική σχισμή (Εικόνα 16).
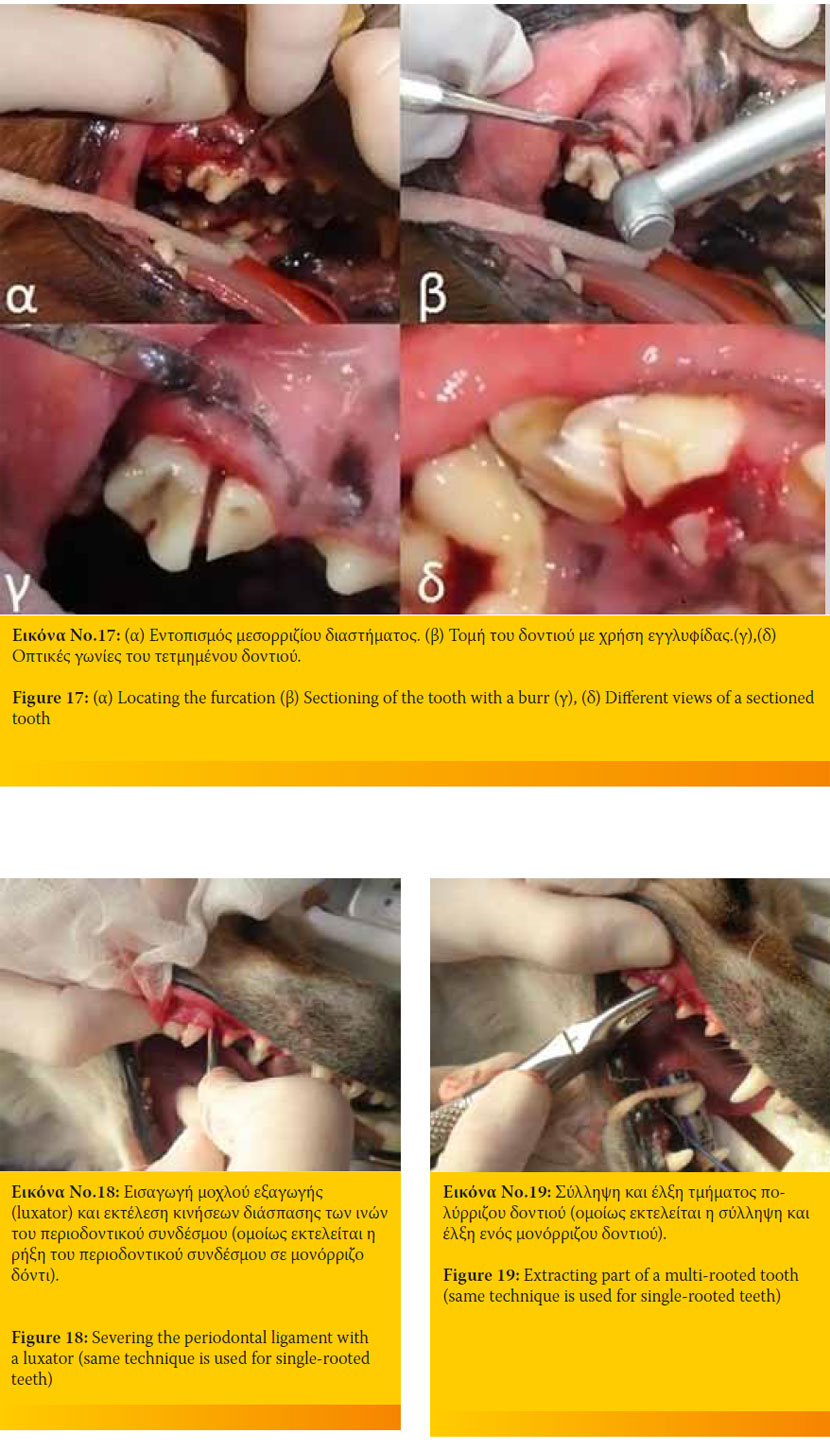
2. Σε περίπτωση που πρόκειται για πολύρριζο δόντι, αφού εντοπιστεί το μεσορρίζιο διάστημα με τη βοήθεια του συνδεσμοτόμου με τον οποίο ανασηκώνονται τα ούλα, διαχωρίζεται το δόντι σε αριθμό τμημάτων ίσο προς τον αριθμό των ριζών του. Στη συνέχεια, το κάθε τμήμα εξάγεται όπως ένα μονόρριζο δόντι (Εικόνα 17).
3. Ακολούθως, εισάγονται με οξεία γωνία και με κατεύθυνση προς της ρίζα του δοντιού στον περιοδοντικό χώρο ευθείς μοχλοί εξαγωγής (luxators εάν υπάρχουν, ή elevators), με την κοίλη επιφάνεια προς την πλευρά του δοντιού και την κυρτή προς το φατνιακό οστό. Ως υπομόχλιο στις κινήσεις εκμόχλευσης του δοντιού θα πρέπει να χρησιμοποιείται το φατνιακό οστό και όχι τα διπλανά δόντια, καθώς υπάρχει κίνδυνος κάκωσης ή και εξαγωγής τους.
4. Εισάγονται όσο το δυνατόν βαθύτερα οι μοχλοί και χρησιμοποιούνται προοδευτικά μεγαλύτερα μεγέθη. Αν στην αρχική φάση της εξαγωγής χρησιμοποιήθηκαν luxators μεταβαίνουμε στους elevators, με τους οποίους μπορεί να ασκηθεί μεγαλύτερη δύναμη χωρίς κίνδυνο θραύσης τους. Ο στόχος της χρήσης των μοχλών είναι αφενός η αύξηση του χώρου μεταξύ ρίζας και φατνίου και αφετέρου η πρόκληση ρήξης των ινών του περιοδοντικού συνδέσμου, με τελικό σκοπό να καταστήσου- με εύσειστο το προς εξαγωγή δόντι (Εικόνα 18).
5. Τελικά, το δόντι ή το τμήμα του δοντιού συλλαμβάνεται με τη χρήση οδοντάγρας ή ριζάγρας και με την άσκηση ελεγχόμενης δύναμης περιστρέφεται ελαφρώς, έλκεται και εξάγεται. Εάν αυτό δεν είναι δυνατό αποφεύγεται η άσκηση μεγαλύτερης δύναμης, αλλά επαναλαμβάνονται τα προηγούμενα βήματα και επιχειρείται εκ νέου έλξη του (Εικόνα 19).
6. Το τραύμα αφήνεται να επουλωθεί κατά β’ σκοπό, ενώ εάν ο λόγος εξαγωγής του δοντιού το επιβάλλει, πραγματοποιείται απόξεση του μετεξακτικού φατνίου με τη βοήθεια κοχλιαρίου ή/και λειαίνεται το χείλος του φατνιακού οστού με τη χρήση κατάλληλης εγγλυφίδας.
Κατά την ανοικτή-χειρουργική τεχνική πραγματοποιούνται τα εξής βήματα:
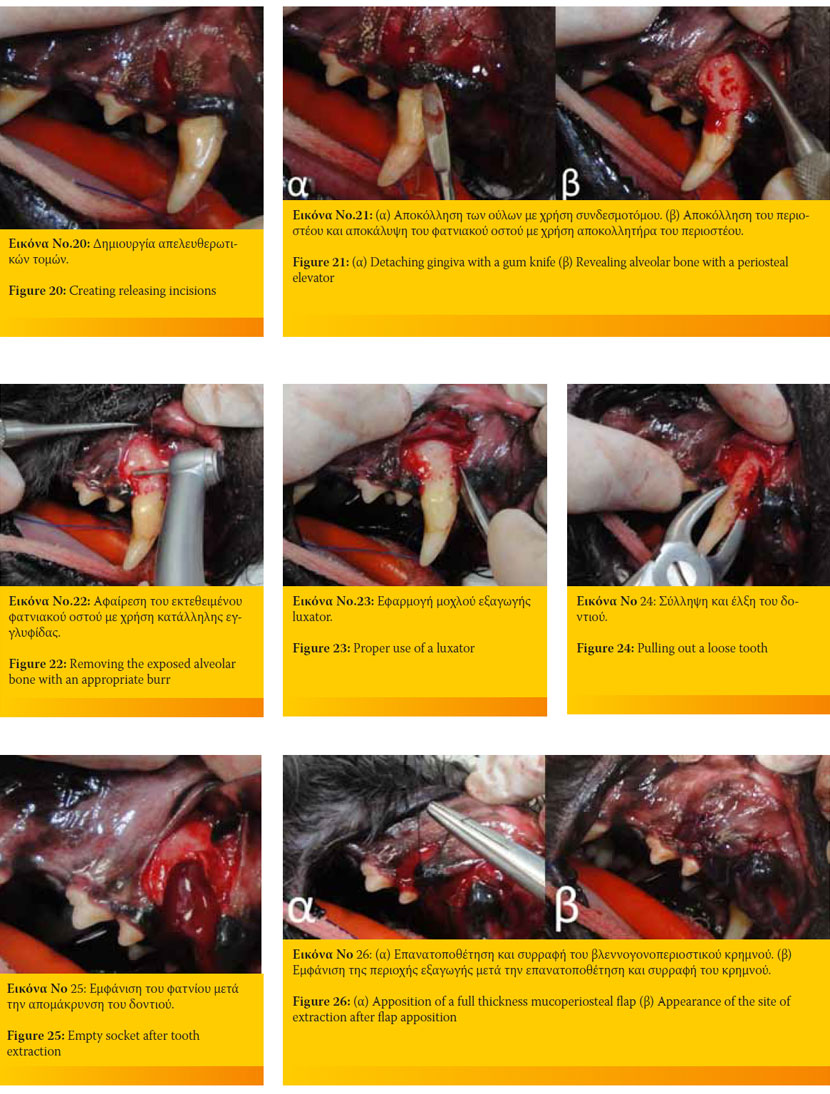
1. Δημιουργούνται με νυστέρι Νο11 ή Νο15 απελευθερωτικές τομές στην παρειακή επιφάνεια των ούλων και του βλεννογόνου, ώστε να παρασκευαστεί βλεννογονοπεριοστκός κρημνός ολικού πάχους. Οι αποκλίνουσες τομές ξεκινούν προσθίως (εγγύς) και οπισθίως (άπω) του δοντιού και επεκτείνονται ώστε η βάση του κρημνού να είναι μεγαλύτερη από το τμήμα του που εμπεριέχει τα ούλα (Εικόνα 20).
2. Ακολούθως, με συνδεσμοτόμο ή νυστέρι αποκολλώνται τα ούλα και με εφαρμογή αποκολλητήρα περιοστέου αποκολλάται το περιόστεο της παρειακής επιφάνειας του φατνιακού οστού, μαζί με τον υπερκείμενο βλεννογόνο, σε έκταση ανάλογη του μεγέθους του κρημνού (Εικόνα 21).
3. Το εκτεθειμένο παρειακό φατνιακό οστό αφαιρείται με τη χρήση κατάλληλης εγγλυφίδας σε χειρολαβή χαμηλών ταχυτήτων (στην περίπτωση αυτή είναι απαραίτητη η συνεχής διαβροχή του με νερό ή φυσιολογικό ορό) ή σε χειρολαβή υψηλών ταχυτήτων με συνεχή παροχή νερού. Το τμήμα του οστού που θα αφαιρεθεί ποικίλει, ανάλογα με την φύση της εξαγωγής (Εικόνα 22).
4. Σε περίπτωση που πρόκειται για πολύρριζο δόντι, αφού εντοπιστεί το μεσορριζικό διάστημα, διαχωρίζεται το δόντι όπως και στην προηγούμενη τεχνική.
5. Εάν κριθεί απαραίτητο δημιουργούνται με εγγλυφίδα εγγύς και άπω του προς εξαγωγή δοντιού δύο «χώροι υποδοχής» για τους μοχλούς εξακτικής (αρχικά luxators εάν υπάρχουν και έπειτα elevators προοδευτικά μεγαλύτερου μεγέθους), ώστε το δόντι ή το τμήμα του δοντιού να καταστεί εύσειστο (Εικόνα 23).
6. Η εξαγωγή του δοντιού ολοκληρώνεται με τη σύλληψη, περιστροφή και έλξη του με τη χρήση οδοντάγρας ή ριζάγρας (Εικόνα 24).
7. Το φατνίο καθαρίζεται και λειαίνεται με τη χρήση κοχλιαρίου απόξεσης ή χειρολαβής χαμηλών ταχυτήτων μετά από προσαρμογή κατάλληλης εγγλυφίδας (Εικόνα 25).
8. Τέλος, ο κρημνός επανατοποθετείται και συρράπτεται προσεκτικά, καθώς συμμετέχει ουσιαστικά στην επούλωση του τραύματος (Εικόνα 26).
Η εξαγωγή δοντιών στη γάτα πραγματοποιείται γενικά με τις ίδιες μεθόδους που εφαρμόζονται στο σκύλο, αλλά πρέπει να λαμβάνεται υπ’ όψιν ότι το κρανίο της γάτας είναι μικρότερο και πιο εύθραυστο από του σκύλου.3,9,10 Τα δόντια της γάτας, επιπλέον, είναι μικρότερου μεγέθους και πιο λεπτής κατασκευής από τα αντίστοιχα ακόμη και μικρόσωμων σκύλων και συνεπώς πιο εύθραυστα.3,9 Από τα παραπάνω εύκολα συμπεραίνεται ότι ο επεμβαίνων επιβάλλεται να είναι ακόμη πιο προσεκτικός, οι χειρισμοί θα πρέπει να είναι πιο ήπιοι, και τα εργαλεία κατάλληλου μεγέθους, ώστε να αποφευχθεί κάταγμα των δοντιών και ιατρογενής τραυματισμός των ιστών της περιοχής. Σε περίπτωση που επιχειρούνται πολλαπλές εξαγωγές (όπως στη χρόνια ουλοστοματίτιδα της γάτας), είναι προτιμότερο να δημιουργείται βλενογγονοπεριοστικός κρημνός και να επιχειρείται χειρουργική εξαγωγή.5
> Επιπλοκές εξαγωγών και αντιμετώπισή τους
Οι συχνότερες επιπλοκές και η αντιμετώπιση τους αναλύονται παρακάτω.
Κάταγμα της ρίζας του δοντιού: Είναι συνήθως αποτέλεσμα άσκησης υπερβολικής δύναμης με το μοχλό εξακτικής ή με την οδοντάγρα.7 Ειδικά εάν το δόντι και το περιοδόντιο δεν είναι υγιή -υπάρχει νέκρωση πολφού, περιοδοντικός θύλακας, οστεόλυση, συρίγγιο, απόστημα κ.α. – τότε κάθε τμήμα της ρίζας πρέπει οπωσδήποτε να απομακρύνεται για να αποτρέπεται η μόλυνση και να διασφαλίζεται η επούλωση.3 Εάν το τμήμα της ρίζας είναι προσπελάσιμο, επιχειρείται η εξαγωγή του αρχικά με τη βοήθεια μοχλών εξακτικής και στη συνέχεια ριζάγρας. Εάν βρίσκεται βαθιά στο φατνίο και η προσπέλασή του είναι δύσκολή, χρησιμοποιείται ανοικτή τεχνική εξαγωγής με δημιουργία βλεννογονοπεριοστικού κρημνού και αφαίρεση τμήματος του φατνιακού οστού με τη βοήθεια κατάλληλης εγγλυφίδας.5
Μετεξακτική αιμορραγία: Αν υπάρξει αιμορραγία που δεν σταματά μετά από λίγα λεπτά, μπορεί να γίνει επικίνδυνη για τη ζωή του ζώου.7 Η αιμορραγία αυτή μπορεί να προέρχεται από το οστό ή τους μαλακούς ιστούς. Η αιμορραγία μπορεί να ελεγχθεί με τους εξής τρόπους:
Α) Απαλή πίεση ή τοποθέτηση ψυχρών επιθεμά- των2,3
Β) Τοποθέτηση αιμοστατικής γάζας ή σπόγγου και συρραφή του φατνίου3,7,9,10
Γ) Ηλεκτροπηξία με διαθερμία2
Δ) Χρήση πολυγαλακτικού οξέος το οποίο βοηθά στη διατήρηση του πήγματος του αίματος στη φατνιακή κοιλότητα, στη γρήγορη επούλωση και στην αποτροπή εμφάνισης οστεΐτιδας μετεξακτικού φατνίου9,10
Στοματορινικό συρίγγιο: δημιουργείται επικοινωνία μεταξύ της στοματικής κοιλότητας και των ρινικών κοιλοτήτων, μπορεί να προέρχεται από τομείς, κυνόδοντες ή προγομφίους της άνω γνάθου, λόγω περιοδοντικής νόσου, περιακρορριζικών αλλοιώσεων ή ακόμη μπορεί να προκληθεί ιατρογενώς κατά την εξαγωγή δοντιού.2,3,7 Η προηγούμενη απώλεια ή εξαγωγή του κυνόδοντα της άνω γνάθου αποτελεί το συχνότερο αίτιο δημιουργίας του στοματορινικού συριγγίου.2,3 Η στοματορινική επικοινωνία αποκαθίσταται χειρουργικά με τη βοήθεια απλού ή διπλού κρημνού ολικού πάχους.3
Κάταγμα της γνάθου: προκαλείται από άσκηση υπερβολικής δύναμης κατά την εξαγωγή ή από αδέξιους χειρισμούς.3 Συχνότερα προκαλείται σε μικρόσωμους και μεσαίου μεγέθους σκύλους ή σε γάτες, κατά την εξαγωγή των κυνοδόντων ή των πρώτων γομφίων της κάτω γνάθου.3,7 Το κάταγμα, κατά κανόνα θα πρέπει να αποκατασταθεί χειρουργικά.3
Τοπική λοίμωξη/οστεομυελίτιδα: Σχετικά σπάνια επιπλοκή της εξαγωγής των δοντιών.9,10 Η οστεΐτιδα του φατνιακού οστού μπορεί να εξελιχθεί περιστασιακά σε οστεομυελίτιδα.32 Αυτό συμβαίνει όταν μειώνεται η αγγειακή παροχή ή όταν η εξαγωγή είναι εξαιρετικά τραυματική, προκαλώντας σημαντική βλάβη των περιοδοντικών ιστών και προδιάθεση σε βακτηριακή μόλυνση.3,9,10 Συνήθως, συνυπάρχει δυσάρεστη οσμή χαρακτηριστική της νέκρωσης. Η υποκείμενη φλεγμονή ευαισθητοποιεί τις νευρικές απολήξεις και οδηγεί σε έντονο πόνο, ο οποίος αντιμετωπίζεται με αναλγητικά φάρμακα.32 Συστήνεται ακόμη, η συστηματική χορήγηση αντιμικροβιακών φαρμάκων, η απομάκρυνση των νεκρωμένων ιστών και η απόξεση του φατνίου μέχρι να αιμορραγήσει και να δημιουργηθεί νέος θρόμβος.2
Τραυματισμός των μαλακών ιστών από το αντίστοιχο δόντι της άλλης γνάθου: παρατηρείται περισσότερο στις γάτες, μετά από εξαγωγή του άνω κυνόδοντα. Όταν εξάγεται ο άνω κυνόδοντας το άνω χείλος έρχεται σε επαφή με τον κάτω κυνόδοντα με αποτέλεσμα να πιέζεται και να τραυματίζεται. Ο κάτω κυνόδοντας μπορεί να τροχιστεί ή ακόμη και να εξαχθεί.3
Ιατρογενείς τραυματισμοί:
Α) Θερμική βλάβη του οστού: προκαλείται από ανεπαρκή ψύξη και υπερθέρμανση της εγγλυφίδας όταν αφαιρείται φατνιακό οστό. Το νεκρωμένο τμήμα του οστού, καθώς και οι νεκρωμένοι μαλακοί ιστοί θα πρέπει να απομακρύνονται. Για να αποφεύγεται η θερμική βλάβη θα πρέπει, ανεξαρτήτως εάν χρησιμοποιείται χειρολαβή υψηλής ή χαμηλής ταχύτητας να ψύχεται επαρκώς η εγγλυφίδα με καταιονισμό νερού ή φυσιολογικού ορού.7
Β) Τραυματισμός των μαλακών ιστών: μικρής έκτασης τραυματισμός των γειτονικών ούλων είναι ήσσονος σημασίας, εκτενέστερος τραυματισμός των μαλακών ιστών οφείλεται συνήθως σε άσκηση υπερβολικής δύναμης κατά τη χρήση των μοχλών εξακτικής και από ολίσθηση των αιχμηρών εργαλείων της εξαγωγής.3 Εάν κριθεί απαραίτητο μπορεί να συρραφούν οι τραυματισμένοι ιστοί.
Γ) Τραυματισμός σε γειτονικό δόντι: η άσκηση μεγάλης πίεσης κατά την εξαγωγή του δοντιού μπορεί να οδηγήσει σε τραυματισμό ή και κάταγμα γειτονικού δοντιού.3 Εάν είναι σημαντική η βλάβη του δοντιού μπορεί να απαιτείται αποκατάστασή του (έμφραξη) ή ακόμη και εξαγωγή του.5
Υπογλώσσιο οίδημα και σιελοκήλη: το οίδημα προκαλείται όταν οι οδοντιατρικοί χειρισμοί είναι βίαιοι3,7 ή όταν διενεργούνται πολλαπλές εξαγωγές στην κάτω γνάθο. Αν το οίδημα είναι έντονο ενδείκνυται η χορήγηση μη στεροειδών αντιφλεγμονωδών φαρμάκων. Η σιελοκήλη (συνήθως βατράχιο) σχηματίζεται αντίστοιχα από τραυματισμό του εκφορητικού πόρου του συμπλέγματος του υπογνάθιου/υπογλώσσιου σιαλογόνων αδένων (έξοδος σάλιου στους υπογλώσσιους ιστούς) κατά την διαδικασία της εξαγωγής του δοντιού.3 Το βατράχιο μπορεί να υποχωρήσει σε κάποιες εβδομάδες, εαν, όμως, επιμένει πρέπει να μαρσιποποιηθεί ή να πραγματοποιηθεί χειρουργική εξαίρεση του συμπλέγματος των σιαλογόνων αδένων.5
Υποβλεννογόνιο και υποδόριο εμφύσημα: δημιουργείται σπάνια, όταν χρησιμοποιείται χειρολαβή υψηλής ταχύτητας κατά την εκτομή του δοντιού ή την απομάκρυνση του φατνιακού οστού, και πιο συχνά όταν χρησιμοποιηθεί αέρας υπό πίεση για αφύγρανση της περιοχής.3,7 Εάν υπάρχει μεγάλο ανοικτό τραύμα στους μαλακούς ιστούς θα πρέπει να συρράπτεται και το εμφύσημα να αφήνεται να απορροφηθεί χωρίς περαιτέρω επέμβαση, το ζώο όμως θα πρέπει να ελέγχεται εάν παρουσιάζει δύσπνοια. Οι ήπιοι χειρισμοί κατά την εξαγωγή συμβάλλουν στην αποφυγή δημιουργίας εμφυσήματος.3
> Μετεγχειρητική αγωγή και φροντίδα
Διαχείριση του πόνου
Για την αντιμετώπιση του πόνου, κρίνεται σκόπιμη η χορήγηση αναλγητικών φαρμάκων για 24-48 ώρες μετά την επέμβαση, αλλά και προεγχειρητικά.5 Μπορούν να χρησιμοποιηθούν ουσίες της κατηγορίας των οπιοειδών και των μη στεροειδών αντιφλεγμονωδών.3,12,17,20,21,23,32,33 Στη μείωση του μετεγχειρητικού άλγους συμβάλει και η εφαρμογή τοπικής αναισθησίας.3,12,17,19,20,21,23,33
Στοματική και σωματική υγιεινή
Η διατήρηση της καλής στοματικής υγιεινής μετά από επεμβάσεις εξαγωγών συμβάλει στην ταχύτερη επούλωση των χειρουργικών τραυμάτων.12 Η μείωση του μικροβιακού φορτίου επιτυγχάνεται με την έκπλυση της στοματικής κοιλότητας προεγχειρητικά με διάλυμα χλωρεξιδίνης και την εφαρμογή γέλης ή πάστας χλωρεξιδίνης για διάστημα 2 εβδομάδων μετεγχειρητικά, 1 ή 2 φορές ημερησίως.3,5,12,14 Μπορεί, επίσης, να βρει εφαρμογή και το ήπιο βούρτσισμα των δοντιών από την 3η-4η μετεγχειρητική ημέρα, αποφεύγοντας όμως τις περιοχές στις οποίες έχουμε επέμβει μέχρι την πάροδο της 1ης εβδομάδας.12 Η χορήγηση αντιμικροβιακών φαρμάκων θα πρέπει να εκτιμάται κατά περίπτωση και εφόσον υπάρχουν επαρκείς λόγοι που την δικαιολογούν, δεδομένου ότι η άσκοπη χρήση μπορεί να οδηγήσει σε ανάπτυξη ανθεκτικών στελεχών ικανών να προκαλέσουν νόσο σε άλλη χρονική στιγμή.10 Η χορήγηση αντιμικροβιακών φαρμάκων, τόσο διεγχειρητικά όσο και μετεγχειρητικά, επιβάλλεται σε περίπτωση που συντρέχουν ιδιαίτεροι λόγοι, όπως νοσήματα τα οποία προκαλούν ανοσοκαταστολή (π.χ. FIV, FeLV στη γάτα)33. Ακόμη, θα πρέπει να χορηγούνται σε ζώα τα οποία πάσχουν από καρδιολογικά νοσήματα ή ενδοκρινοπάθειες, όταν πραγματοποιούνται πολλαπλές εξαγωγές και ειδικά όταν αυτές πραγματοποιούνται λόγω εκτεταμένης περιοδοντικής νόσου ή σε εξαγωγή δοντιών τα οποία είναι υπαίτια για τη δημιουργία αποστήματος ή συριγγίου5,14. Συχνότερα χορηγούνται η κλινδαμυκίνη, η μετρονιδαζόλη και η αμοξικιλλίνη – κλαβουλανικό κάλιο.5,10
Διατροφή
Νερό μπορεί να χορηγηθεί στο ασθενές ζώο, αμέ- σως μόλις ανανήψει από την γενική αναισθησία.3 Συστήνεται για 7-10 ημέρες η χορηγούμενη τροφή να είναι μαλακής σύστασης και σε θερμοκρασία δωματίου, ενώ καλό είναι να αποφεύγονται τα γαλακτοκομικά προϊόντα για 2-3 ημέρες (μπορούν να λειτουργήσουν ως υπόστρωμα για την ανάπτυξη παθογόνων βακτηρίων)5. Ακόμη, για διάστημα μιας εβδομάδας συστήνεται να αποφεύγεται το παιχνίδι του ζώου με σκληρά αντικείμενα, προκειμένου να αποφευθεί κάποια αιμορραγία ή η ρήξη των ραμμάτων εάν έχουν τοποθετηθεί.3,12 Συνήθως, τα περισσότερα ζώα καταναλώνουν νερό και τροφή ακόμα και μετά από πολλαπλές εξαγωγές την πρώτη ή τη δεύτερη μετεγχειρητική ημέρα,3,5 ώστε η ανάγκη για υποχρεωτική σίτιση ή τοποθέτηση οισοφαγικού καθετήρα διατροφής να μη θεωρείται συχνή.3,12,33
> Μετεγχειρητική αξιολόγηση και παρακολούθηση
Ο ιδιοκτήτης θα πρέπει να παρακολουθεί το κατοικίδιο του για αιμορραγία (η παρουσία αιμορραγικού σάλιου θωρείται φυσιολογική τα πρώτα δύο εικοσιτετράωρα), ενδείξεις πόνου όπως ληθαργικότητα και ανορεξία, δύσοσμη αναπνοή, και να το προσκομίσει για επανεξέταση σε 1-2 εβδομάδες ώστε να αξιολογηθεί η πορεία της επούλωσης.5,12,14,33 Αυτή η επίσκεψη, εξάλλου, θα μπορούσε να αποτελέσει και μια ευκαιρία συζήτησης με τον ιδιοκτήτη για την πρόληψη των παθήσεων και τα ωφέλη του βουρτσίσματος των δοντιών, καθώς και της περιποίησης και του τακτικού ελέγχου της στοματικής κοιλότητας από τον ίδιο.5,12,14
> Βιβλιογραφία
1. Bellows J. Oral Surgical Equipment, Materials, and Techniques. In: Small Animal Dental Equipment, Materials and Techniques, A Primer. 1st edn. Blackwell Publishing: Oxford, UK, 2004, pp. 297-362.
2. Marreta SM, Tholen M. Extraction Techniques and Management of Associated Complications. In: Small Animal Oral Medicine and Surgery. Bojrab MJ, Tholen M (ed.). Lea and Febiger: Philadelphia, USA, 1990, pp. 75-94.
3. Reiter AM. Dental Surgical Procedures. In: BSAVA Manual of Canine and Feline Dentistry. Tutt C, Deeprose J, Crossley D (ed). 3rd edn. BSAVA: Quedgeley, UK, 2007, pp. 178-195.
4. Kesel LM. Assisting with Extractions. In: Veterinary Dentistry for the Small Animal Technician. 1st edn. Iowa State University Press: Ames, 2000, pp. 141-155.
5. Παπαδημητρίου Σ. Ενδείξεις και τεχνικές εξαγωγής δοντιών. Πανεπιστημιακές παραδόσεις 7ου εξαμήνου. Τμήμα Κτηνιατρικής Α.Π.Θ: Θεσσαλονίκη, 2014.
6. Tutt C. Exodontics. In: Small Animal Dentistry, A Manual of Techniques. Blackwell Publishing: Oxford, UK, 2006, pp. 131-171.
7. Gorrel C. Tooth Extraction. In: Veterinary Dentistry for the General Practitioner, 1st edn Saunders of Elsevier: Philadelphia, USA, 2004, pp. 157-174.
8. Holmstrom SE, Frost PF, Eisner ER. Exodontics. In: Veterinary Dental Techniques for the Small Animal Practitioner. 5th edn, Mosby Inc.: Philadelphia, 2007, pp. 291-338.
9. Harvey CE, Emily PP. Oral surgery. In: Small Animal Dentistry. Mosby-Year Book Inc.: St.Louis, 1993, pp. 312- 377.
10. Harvey CE. Basic Techniques-Extraction and Antibiotic Treatment. In: BSAVA Manual of Small Animal Dentistry. Harvey CE, Orr SH (ed). BSAVA: Cheltenham, 1990, pp. 29-35.
11. Holmstrom SE. Exodontics. In: Veterinary Dentistry, A Team Approach. 2nd edn. Elsevier Saunders: St. Louis, 2013, pp. 288-304.
12. Lommer MJ. Principles of Exodontics. In: Oral and Maxillofacial Surgery in Dogs and Cats. Verstraete FJM, Lommer MJ (ed). Saunders of Elsevier: Philadelphia, USA, 2012 pp. 97-114.
13. Holmstrom SE, Frost PF, Eisner ER. Exodontics. In: Veterinary Dental Techniques for the Small Animal Practitioner. 3rd edn. Saunders of Elsevier: Philadelphia, USA, 2004, pp. 291-338.
14. Lommer MJ, Verstraete FJM. Simple Extraction of Single-Rooted Teeth. In: Oral and Maxillofacial Surgery in Dogs and Cats.Verstraete FJM, Lommer MJ (ed). Saunders of Elsevier: Philadelphia, USA, 2012, pp. 115- 120.
15. Lommer MJ, Tsugawa AJ, Verstraete FJM. Extraction of Multirooted Teeth in Dogs. In: Oral and Maxillofacial Surgery in Dogs and Cats. Verstraete FJM, Lommer MJ (ed). Saunders of Elsevier: Philadelphia, USA, 2012, pp. 131-139.
16. Joubert K, Tutt C. Anaesthesia and Analgesia. In: BSAVA, Manual of Canine and Feline Dentistry. Tutt C, Deeprose J, Crossley D (ed). 3rd edn. BSAVA: Quedgeley, UK, 2007, pp. 41-55.
17. Tutt C. Pain Management. In: Small Animal Dentistry, A Manual of Techniques, Blackwell Publishing: Oxford, UK, 2006, pp. 229-238.
18. Kesel LM. Anesthesia, Analgesia and Postsurgical Support. In: Veterinary Dentistry for the Small Animal Technician. 1st edn. Iowa State University Press: Ames, 2000, pp. 101-120.
19. Gorrel C. Anesthesia and Analgesia. In: Veterinary Dentistry for the General Practitioner. Saunders of Elsevier: Philadelphia, USA, 2004, pp. 11-22.
20. Holmstrom SE, Frost PF, Eisner ER. Anesthesia and Pain Management in Dental and Oral Procedures. In: Veterinary Dental Techniques for the Small Animal Practitioner. 3rd edn. Saunders of Elsevier: Philadelphia, USA, 2004, pp. 601-624.
21. Pascoe PJ. Anesthesia and Pain Management. In: Oral and Maxillofacial Surgery in Dogs and Cats. Verstraete FJM, Lommer MJ (ed), Saunders of Elsevier: Philadelphia, USA, 2012, pp. 23-42.
22. Holmstrom SE. Local Anesthesia. In: Veterinary Dentistry, A Team Approach. 2nd edn. Saunders of Elsevier: St. Louis, 2013, pp. 135-149.
23. Bellows J. Local and Regional Anesthesia and Pain Control. In: Small Animal Dental Equipment, Materials and Techniques. A Primer. 1st Edn. Blackwell Publishing: Oxford, UK, 2004, pp. 105-114.
24. Holmstrom SE. The Complete Prophy. In: Veterinary Dentistry, A Team Approach. 2nd edn. Saunders of Elsevier: St. Louis, 2013, pp. 167-193.
25. Gorrel C. Equipment and Instrumentation. In: Veterinary Dentistry for the General Practitioner, 1st edn. Saunders of Elsevier: Philadelphia, USA, 2004, pp. 1-10.
26. Robinson J. Dental Instrumentation and Equipment. In: BSAVA, Manual of Canine and Feline Dentistry. Tutt C, Deeprose J, Crossley D (ed). 3rd edn. BSAVA: Quedgeley, UK, 2007, pp. 67-76.Holmstrom SE, Frost PF, Eisner ER. Dental Equipment and Care. In: Veterinary Dental Techniques for the Small Animal Practitioner. 3rd edn. Saunders of Elsevier: Philadelphia, USA, 2004, pp. 39-130.
27. Marreta SM (απόδοση στην ελληνική γλώσσα: Παπαδημητρίου ΣΑ, Ράλλης Τ). Οδοντιατρική και πα- θήσεις της στοματικής κοιλότητας και του φάρυγγα. In: Saunders Εγχειρίδιο Κτηνιατρικής των Μικρών Ζώων. 3rd edn. Mendor Editions S.A.: 2008, pp. 609-635.
28. Deeprose J. Operator Safety and Health Considerations. In: BSAVA Manual of Canine and Feline Dentistry. Tutt C, Deeprose J, Crossley D (ed). 3rd edn. BSAVA: Quedgeley, UK, 2007, pp. 56-66.Holmstrom SE, Holmstrom LA. Personal Safety and Ergonomics. In: Veterinary Dentistry, A Team Approach. 2nd edn. Saunders of Elsevier: St. Louis, 2013, pp. 117-134.
29. Gorrel C. Antibiotics and Antiseptics. In: Veterinary Dentistry for the General Practitioner, 1st edn. Saunders: Philadelphia, USA, 2004, pp. 23-28.
30. Crossley DA, notes for the British Veterinary Dental Association’s (BVDA), Basic Dentistry Courses, 2003.
31. Lommer MJ. Special Considerations in Feline Exodontics. In: Oral and Maxillofacial Surgery in Dogs and Cats. Verstraete FJM, Lommer MJ (ed). Saunders of Elsevier: Philadelphia, USA, 2012, pp. 141-152.