> Περίληψη
Η κήλη του οισοφαγικού τρήματος εμφανίζεται σπάνια στο σκύλο και σπανιότερα στη γάτα. Η ολισθαίνουσα κήλη είναι η συχνότερη στην κλινική πράξη. Η αιτιολογία και η παθοφυσιολογία της κήλης του οισοφαγικού τρήματος δεν είναι πλήρως γνωστές. Η φυλή Shar-pei παρουσιάζει προδιάθεση στην εμφάνιση της κήλης. Το μεγαλύτερο μέρος της συμπτωματολογίας οφείλεται στη γαστροοισοφαγική παλινδρόμηση. Η διάγνωση τίθεται μετά από οισοφαγοσκόπηση, εναλ- λακτικά ο απεικονιστικός έλεγχος μπορεί να δώσει χρήσιμες πληροφορίες και η αντιμετώπιση μπορεί να είναι φαρμακευτική ή χειρουργική. Σκοπός της χειρουργικής θεραπείας είναι η ανατομική αποκατάσταση και σταθεροποίηση της κήλης. Η πρόγνωση είναι συνήθως ευνοϊκή.
Σκοπός αυτής της ανασκόπησης είναι η περιγραφή της αιτιολογίας, παθοφυσιολογίας και αντιμετώπισης της κήλης του οισοφαγικού τρήματος στα ζώα συντροφιάς.
> ΤΑΞΙΝΟΜΗΣΗ
Κήλη του οισοφαγικού τρήματος ή οισοφαγοκήλη (ΚΟΤ) ονομάζεται η πρόπτωση ενδοκοιλιακών οργάνων, διαμέσου του οισοφαγικού τρήματος, στη θωρακική κοιλότητα. Η ΚΟΤ παρατηρείται σπάνια στο σκύλο και σπανιότερα στη γάτα. 1, 2 Έχουν περιγραφεί 4 τύποι ΚΟΤ. Η ταξινόμηση της ΚΟΤ στα ζώα συντροφιάς χαρακτηρίζεται από ασάφεια αλλά ακολουθεί αυτήν του ανθρώπου.1-5
Τύπος Ι
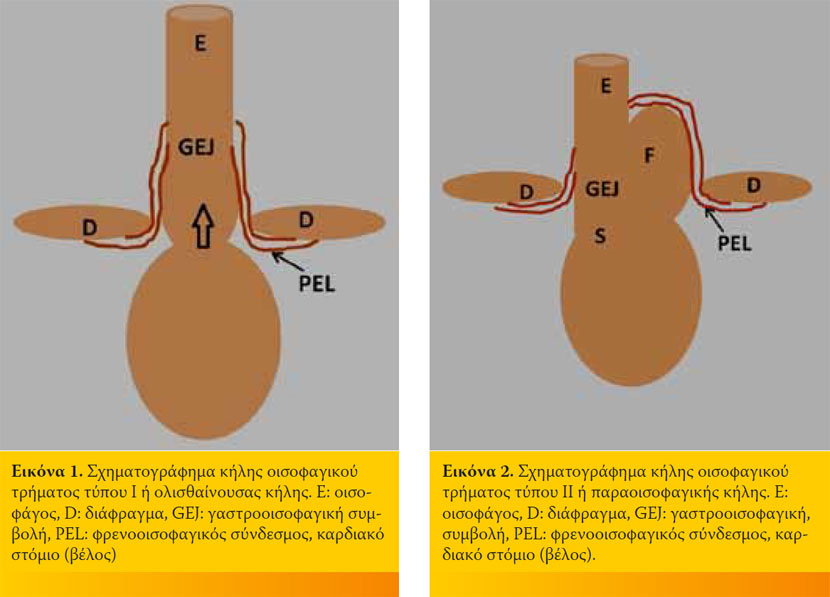
Ο τύπος I ή ολισθαίνουσα ΚΟΤ χαρακτηρίζεται από τη δυναμική και διαλείπουσα πρόπτωση της ενδοκοιλιακής μοίρας του οισοφάγου όπου αυτή υφίσταται, της γαστροοισοφαγικής συμβολής και τμήματος του στομάχου, διαμέσου του οισοφαγικού τρήματος, στη θωρακική κοιλότητα (Εικόνα 1). Η ολισθαίνουσα ΚΟΤ συναντάται συχνότερα από τους υπόλοιπους τύπους στα ζώα συντροφιάς και αποτελεί τον συχνότερο τύπο ΚΟΤ που έχει περιγραφεί στη γάτα.6-24
Τύπος ΙΙ
Ο τύπος ΙΙ ή παραοισοφαγική ΚΟΤ χαρακτηρίζεται από την πρόπτωση του θόλου του στομάχου, στη θωρακική κοιλότητα, κατά μήκος της ενδοθωρακικής μοίρας του οισοφάγου, ενώ η γαστροοισοφαγική συμβολή παραμένει στη θέση της (Εικόνα 2). Η παραοισοφαγική κήλη έχει περιγραφεί σε 3 σκύλους.25-27 Παραοισοφαγική κήλη με πρόπτωση μόνο του επιπλόoυ στη θωρακική κοιλότητα περιγράφηκε σε μια γάτα. 28
Τύπος ΙΙΙ
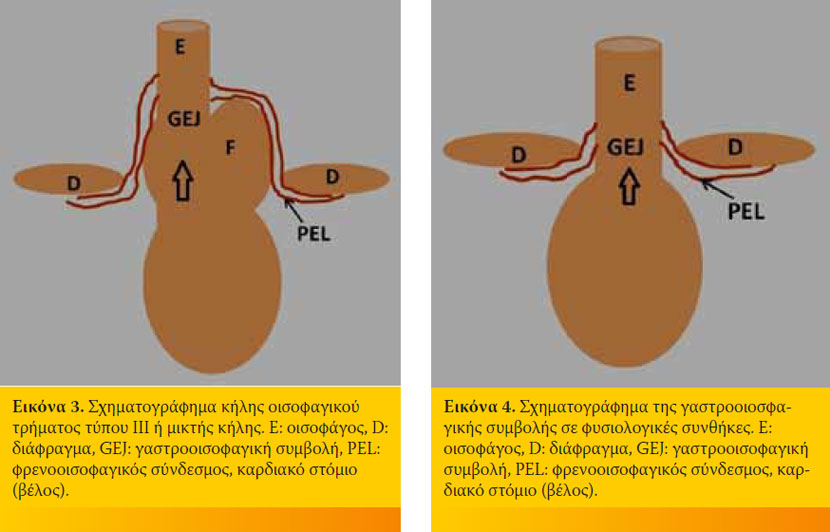
Ο τύπος ΙΙΙ ή μικτή ΚΟΤ συνδυάζει τα χαρακτηριστικά των 2 προηγούμενων μορφών ΚΟΤ Ι και ΙΙ και έχει περιγραφεί σε 2 σκύλους (Εικόνα 3).4, 29
Τύπος IV
Ο τύπος IV αποτελεί μια ΚΟΤ τύπου ΙΙΙ που συνοδεύεται από την πρόπτωση του στομάχου, του ήπατος ή άλλων ενδοκοιλιακών οργάνων στη θωρακική κοιλότητα και έχει περιγραφεί σε 3 σκύλους. 30-32 Γενικά η ΚΟΤ μπορεί να έχει μόνιμο ή δυναμικό χαρακτήρα ανάλογα με τις μεταβολές της θέσης του ζώου και της ενδοθωρακικής πίεσης.1 Η γνώση των διαφόρων τύπων της ΚΟΤ είναι απαραίτητη επειδή κάθε τύπος συνοδεύεται από διαφορετική παθοφυσιολογία και συμπτωματολογία που απαιτεί διαφορετική θεραπεία.3,4, 25
> ΧΕΙΡΟΥΡΓΙΚΗ ΑΝΑΤΟΜΙΚΗ ΚΑΙ ΛΕΙΤΟΥΡΓΙΚΗ ΥΠΟΜΝΗΣΗ ΤΗΣ ΓΑΣΤΡΟΟΙΣΟΦΑΓΙΚΗΣ ΣΥΜΒΟΛΗΣ
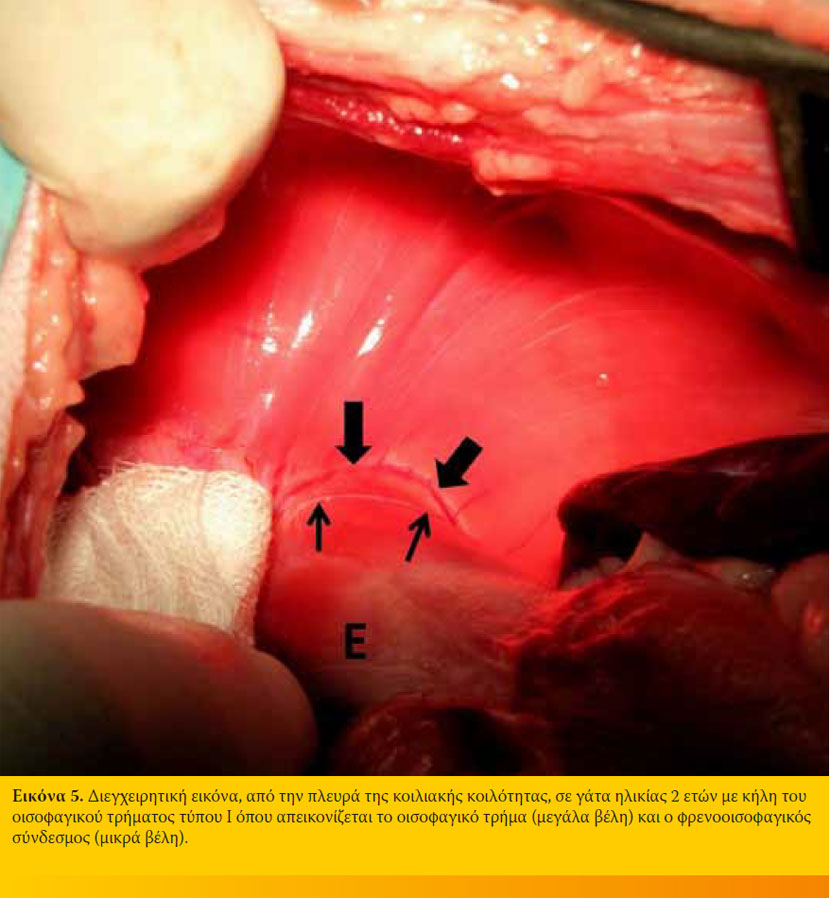
Το οισοφαγικό τρήμα είναι ένα άνοιγμα του διαφράγματος, που βρίσκεται κοιλιακά του αορτικού τρήματος και δεξιά της μέσης γραμμής, από το οποίο διέρχεται ο οισοφάγος για να εισέλθει στην κοιλιακή κοιλότητα. Η γαστροοισοφαγική συμβολή αποτελεί την ανατομική περιοχή μετάπτωσης του οισοφάγου στο στόμαχο, που φυσιολογικά βρίσκεται στην ενδοκοιλιακή μοίρα του οισοφάγου. Ο οισοφάγος συνδέεται με το οισοφαγικό τρήμα διαμέσου της φρενοοισοφαγικού συνδέσμου που εμποδίζει την μετακίνηση του ενδοκοιλιακού οισοφάγου προς τη θωρακική κοιλότητα (Εικόνα 4). Στη γάτα ο φρενοοισοφαγικός σύνδεσμος διαφέρει από αυτόν του σκύλου στο ότι το κατωφερές τμήμα του συνδέεται με τον οισοφάγο πίσω από την καρδιοοισοφαγική γωνία και οι οισοφαγικές συνδέσεις του είναι περισσότερο χαλαρές (Εικόνα 5).33 Ο οπίσθιος οισοφαγικός σφικτήρας αποτελεί ζώνη υψηλής πίεσης, και όχι διακριτή ανατομική περιοχή, που εκτείνεται από το οισοφαγικό τρήμα μέχρι το καρδιακό στόμιο του στομάχου τόσο στο σκύλο όσο και στη γάτα. 34,35 Ο οπίσθιος οισοφαγικός σφικτήρας του σκύλου αποτελείται ιστολογικά από γραμμωτές μυικές ίνες, ενώ της γάτας από λείες μυϊκές ίνες. 33
Υποστηρίζεται ότι η ενδοκοιλιακή μοίρα του οισοφάγου δέχεται μεγαλύτερη εξωαυλική πίεση με αποτέλεσμα να παρεμποδίζεται η γαστροοισοφαγική παλινδρόμηση (ΓΟΠ). Η άποψη όμως αυτή αμφισβητείται στο σκύλο αφού αποδείχθηκε ότι μερικές φυλές στερούνται της ενδοκοιλιακής μοίρας του οισοφάγου. 36,37 Για τη γάτα δεν είναι ακόμη γνωστό αν υφίσταται ενδοκοιλιακή μοίρα του οισοφάγου. Η διατήρηση της υψηλής πιέσεως και η αποτροπή της ΓΟΠ θεωρείται ότι ελέγχεται από διάφορους εξωγενείς παράγοντες όπως το μικρό μήκος της ενδοκοιλιακής μοίρας του οισοφάγου, το δεξιό σκέλος του διαφράγματος που περιβάλλει την ενδοκοιλιακή μοίρα του οισοφάγου ως λάσο, τον φρενοοισοφαγικό σύνδεσμο, το καρδιακό στόμιο του στομάχου, τη διατήρηση οξείας της καρδιοοισοφαγικής γωνίας και τη θέση κατάκλισης του σκύλου. 3, 36, 38
> ΑΙΤΙΟΛΟΓΙΑ, ΠΑΘΟΦΥΣΙΟΛΟΓΙΑ ΚΑΙ ΠΡΟΔΙΑΘΕΤΙΚΟΙ ΠΑΡΑΓΟΝΤΕΣ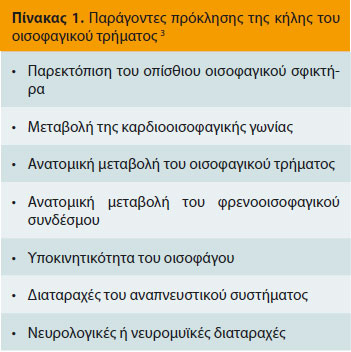 Η κήλη του οισοφαγικού τρήματος είναι μια παθο λογική κατάσταση, με όχι πλήρως διευκρινισμένη αιτιολογία και παθοφυσιολογία, που χαρακτηρίζεται από αλληλεπίδραση πολλών παραγόντων (Πίνακας1).3 Οι περισσότερες πληροφορίες που έχουμε για την παθοφυσιολογία της ΚΟΤ στα ζώα συντροφιάς αντλούνται από μελέτες στον άνθρωπο, ενώ υποστηρίζεται ότι η παθοφυσιολογία του σκύλου και του ανθρώπου είναι παρόμοιες. 3
Η κήλη του οισοφαγικού τρήματος είναι μια παθο λογική κατάσταση, με όχι πλήρως διευκρινισμένη αιτιολογία και παθοφυσιολογία, που χαρακτηρίζεται από αλληλεπίδραση πολλών παραγόντων (Πίνακας1).3 Οι περισσότερες πληροφορίες που έχουμε για την παθοφυσιολογία της ΚΟΤ στα ζώα συντροφιάς αντλούνται από μελέτες στον άνθρωπο, ενώ υποστηρίζεται ότι η παθοφυσιολογία του σκύλου και του ανθρώπου είναι παρόμοιες. 3
Στους σκύλους με ΚΟΤ η γαστροισοφαγική συμβολή μετατοπίζεται προς τα εμπρός με αποτέλεσμα τη διαταραχή των εξωγενών παραγόντων που ελέγχουν την πίεση του οπίσθιου οισοφαγικού σφικτήρα και την πρόκληση οισοφαγίτιδας από ΓΟΠ στην ποία οφείλεται και η συμπτωματολογία της ΚΟΤ. Ωστόσο παραμένει άγνωστο γιατί πολλά ζώα συντροφιάς με ΚΟΤ παραμένουν ασυμπτωματικά. 12,16 Πιθανόν η ύπαρξη προστατευτικών μηχανισμών που προλαμβάνουν την οισοφαγίτιδα όπως ο μικρός χρόνος έκθεσης του οισοφαγικού αυλού στο περιεχόμενο της παλινδρόμησης, η εξουδετέρωση του περιεχομένου από τα διττανθρακικά του σίαλου και η ιστολογική δομή του οισοφαγικού βλεννογόνου φαίνεται να είναι ισχυρότερη σε αυτά τα ζώα. 39 Επιπλέον στο σκύλο, αντίθετα με ότι πιστεύονταν παλαιότερα, δεν υφίσταται πρωτογενής ανεπάρκεια (αχαλασία) του οπίσθιου οισοφαγικού σφικτήρα.3 Η συγγενής μορφή ΚΟΤ και ειδικότερα η τύπου Ι είναι η συχνότερη και παρατηρείται στις βραχυκεφαλικές φυλές και ειδικά στα Αγγλικά bulldog και στα Shar-pei και πιθανόν να οφείλεται σε μη φυσιολογική σύγκλειση του διαφράγματος κατά την εμβρυική ζωή.15,16,18,22,40-42 Στις βραχυκεφαλικές φυλές βρέθηκε ισχυρή συσχέτιση μεταξύ απόφραξης του ανώτερου αναπνευστικού και οισοφαγίτιδας από ΓΟΠ.41,42 Η εισπνευστική δύσπνοια που παρατηρείται στις βραχυκεφαλικές φυλές, κυρίως στα Αγγλικά bulldog, αλλά και σε άλλες φυλές σκύλων και γατών εξαιτίας της απόφραξης του ανώτερου αναπνευστικού συστήματος θα μπορούσε να προκαλέσει αύξηση της αρνητικής ενδοοισοφαγικής και της ενδοϋπεζωκοτικής πίεσης με συνέπεια την πρόκληση ΚΟΤ και τη μετακίνηση της γαστροισοφαγικής συμβολής και του στομάχου στη θωρακική κοιλότητα και την εμφάνιση σχετικής συμπτωματολογίας.10,18,24,41-44 Η ΚΟΤ επίσης μπορεί να εμφανιστεί ως επιπλοκή της χειρουργικής αποκατάστασης της διαφραγματοκήλης λόγω κάκωσης ή αυξημένης πίεσης στην περιοχή του οισοφαγικού τρήματος και σε μεταβολές της δραστηριότητας του πνευμονογαστρικού λόγω χειρουργικού τραυματισμού του. 10,12,13,17 Περιστατικά με τέτανο στο σκύλο συσχετίστηκαν με την εμφάνιση ΚΟΤ λόγω νευρομυϊκής δυσλειτουργίας του διαφράγματος, της γαστροοισοφαγικής συμβολής και του κοιλιακού τοιχώματος με αποτέλεσμα το σπασμό του διαφράγματος, την υποκινητικότητα του οισοφάγου και την εμφάνιση ΚΟΤ.45,46 Η ΚΟΤ μπορεί επίσης να σχετίζεται με την εμφάνιση υποκινητικότητας του οισοφάγου, μεγαοισοφάγου ή ακόμη και στένωσης του αυλού του, εξαιτίας της οισοφαγίτιδας από ΓΟΠ, τόσο στο σκύλο όσο και στη γάτα.12,13,15,16,18,19 Αναφορικά με την κήλη τύπου ΙΙ ή παραοισοφαγική κήλη αυτή σπάνια συνοδεύεται από οισοφαγίτιδα λόγω ΓΟΠ εκτός αν συνυπάρχει με ολισθαίνουσα κήλη ή με μεγαοισοφάγο (τύποι ΙΙΙ και IV).4,26,27,32
> ΚΛΙΝΙΚΗ ΕΙΚΟΝΑ
Οι περισσότεροι σκύλοι με συγγενή ΚΟΤ εμφανίζουν συμπτώματα σε ηλικία μικρότερη των 12 μηνών, ενώ στις γάτες η διάγνωση γίνεται συχνότερα σε ηλικία μεγαλύτερη των 12 μηνών.10,12,15,22 Σε μερικά ζώα η ΚΟΤ δεν δίνει κλινική συμπτωματολογία.12,16 Σε ΚΟΤ τύπου Ι η κλινική εικόνα σχετίζεται συχνότερα με τη ΓΟΠ και περιλαμβάνει αναγωγές, εμέτους, σιαλόρροια, αιματέμεση, απώλεια βάρους και αναπνευστική δυσχέρεια. 10,12,15,22 Σε ΚΟΤ τύπου II-IV η κλινική εικόνα περιλαμβάνει συχνότερα αναπνευστική δυσχέρεια, κατάπτωση ή κατάρρευση.25-27,30,32 Σε σκύλο Shar-pei με ΚΟΤ τύπου IV διαπιστώθηκε σύνδρομο Budd-Chiari λόγω συμπίεσης της οπίσθιας κοίλης φλέβας από τον μετατοπισμένο αριστερό ηπατικό λοβό.31
> ΔΙΑΓΝΩΣΗ
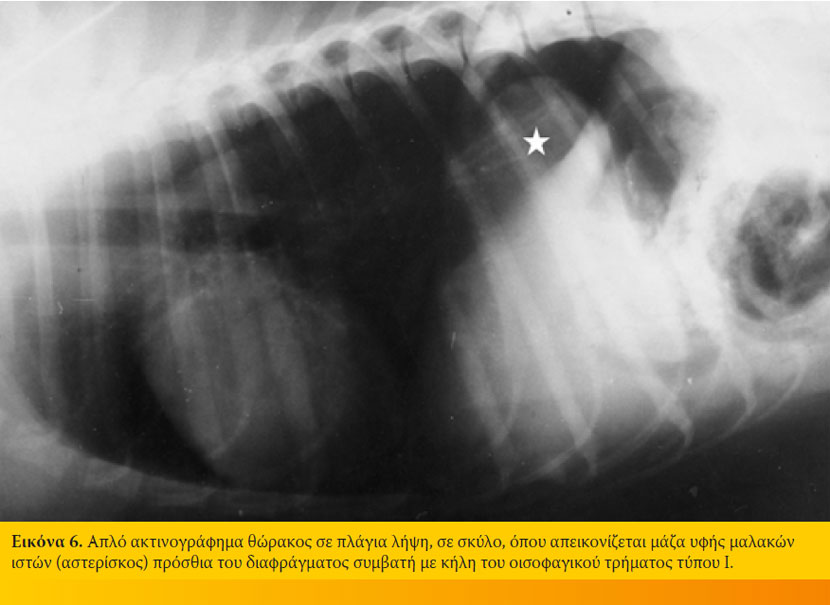
Η επιβεβαίωση της διάγνωσης γίνεται με ακτινολογικό έλεγχο του θώρακα και οισοφαγογράφημα με ή χωρίς ακτινοσκόπηση μετά από λήψη βαριούχου γεύματος.2,10,12,15,16 Στα απλά ακτινογραφήματα του θώρακα διαπιστώνεται μάζα υφής μαλακών ιστών ή μάζα με αερώδη συλλογή στο οπίσθιο τμήμα της θωρακικής μοίρας του οισοφάγου (επιφρενική μάζα), μεγαοισοφάγος και εισροφητική βρογχοπνευμονία (Εικόνα 6).10,12,15,16
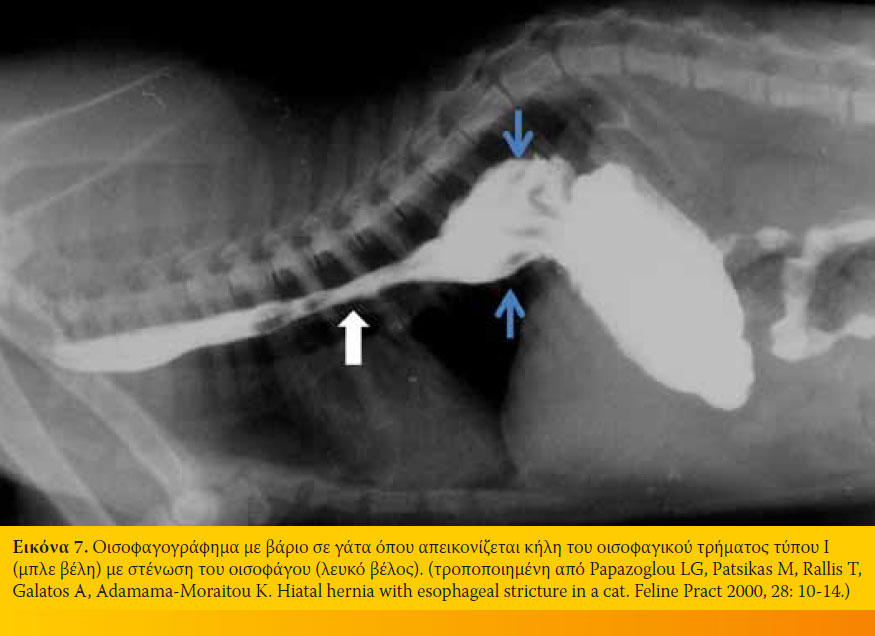
Η διαφορική διάγνωση θα πρέπει να περιλαμβάνει το εκκόλπωμα του οισοφάγου, το γαστροοισοφαγικό εγκολεασμό, τα νεοπλάσματα και τα ξένα σώματα.2 Το οισοφαγογράφημα μετά από λήψη βαριούχου γεύματος μπορεί να βοηθήσει στη διαφορική διάγνωση της ΚΟΤ τύπου I από την II και θα δείξει πρόσθια μετατόπιση της γαστροοισοφαγικής συμβολής, κατακράτηση του βαρίου στην διατεταμένη οπίσθια μοίρα του οισοφάγου και απεικόνιση των πτυχών του στομάχου (Εικόνα 7). 10,12,15,16 Στο οισοφαγογράφημα με ακτινοσκόπηση θα φανεί η ΓΟΠ, η μετατόπιση της γαστροοισοφαγικής συμβολής και η υποκινητικότητα του οισοφάγου.12,15,16 Η οισοφαγοσκόπηση με εύκαμπτο ενδοσκόπιο μας βοηθάει να δούμε τη διάταση του οισοφαγικού τρήματος, την οισοφαγίτιδα και τη ΓΟΠ.2
> ΘΕΡΑΠΕΙΑ
Συντηρητική αγωγή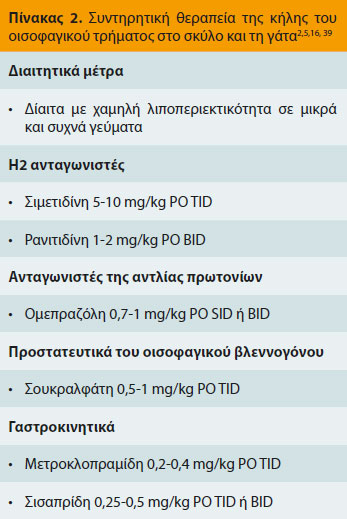 Ο τύπος Ι συγγενούς ΚΟΤ μπορεί να αντιμετωπιστεί τόσο συντηρητικά όσο και χειρουργικά με πολύ καλά αποτελέσματα.11,12,14-16,22 Υπάρχει διχογνωμία όμως μεταξύ των χειρουργών σχετικά με την απόφαση για χειρουργική ή συντηρητική αντιμετώπιση. Μερικοί χειρουργοί προτείνουν άμεση χειρουργική αντιμετώπιση στη φυλή sharpei αφού τα περισσότερα ζώα της φυλής αυτής φαίνεται να μην ανταποκρίνονται στη συντηρητική αγωγή.15,22,47 Η αντιμετώπιση πάντως της πρωτογενούς αιτίας συμβάλει στην υποχώρηση των συμπτωμάτων.2,41,42 Η συντηρητική αγωγή γενικότερα στοχεύει στην αντιμετώπιση των συμπτωμάτων της οισοφαγίτιδας από ΓΟΠ. Ειδικότερα οι στόχοι της συντηρητικής αγωγής περιλαμβάνουν την ελάττωση του όγκου του υγρού της παλινδρόμησης, της έκκρισης και την αύξηση του pH του γαστρικού υγρού, την προστασία του οισοφαγικού βλεννογόνου από την δράση του παλινδρομούντος υγρού και την επιτάχυνση της γαστρικής κένωσης με τη σύγχρονη αύξηση του τόνου του οπίσθιου οισοφαγικού σφικτήρα.2,12,16 Αυτό επιτυγχάνεται με τη χορήγηση δίαιτας με χαμηλά λιπαρά σε συχνά γεύματα, τη χορήγηση Η2 αναστολέων ή αναστολέων της αντλίας πρωτονίων, γαστροπροστατευτικών και γαστροκινητικών. Σε περίπτωση μεγαοισοφάγου η χορήγηση τροφής θα πρέπει να γίνεται από ύψος. Οι δραστικές ουσίες που χρησιμοποιούνται για τη συντηρητική αγωγή της ΚΟΤ και η δοσολογία τους περιγράφονται στον πίνακα 2. Η συντηρητική αγωγή διαρκεί 30 ημέρες και μόνο σε περίπτωση που τα αποτελέσματά της είναι πτωχά συνιστάται η χειρουργική αντιμετώπιση. Η απόφαση πάντως για το ποια αγωγή θα δοθεί στη συνέχεια πρέπει να λαμβάνεται σε εξατομικευμένη βάση.3,12,16 Σύμφωνα με μια μελέτη 8 από τους 15 σκύλους και γάτες με συγγενή ΚΟΤ τύπου Ι που αντιμετωπίστηκαν συντηρητικά εμφάνισαν ίαση.16 Στα ζώα που δεν έχουν κλινική συμπτωματολογία δεν απαιτείται καμία θεραπεία.12 Στην κήλη τύπου ΙΙ δεν παρατηρείται ΓΟΠ αφού ο οπίσθιος οισοφαγικός σφικτήρας παραμένει στη θέση του. Στον τύπο αυτό η συμπτωματολογία οφείλεται στη πρόπτωση του στομάχου ή άλλων σπλάχνων στην θωρακική κοιλότητα και επομένως απαιτείται πάντοτε χειρουργική θεραπεία.25,26,28 Η παρουσία όμως μεγαοισοφάγου και κατά συνέπεια ΓΟΠ αποτελεί εξαίρεση και επιβάλει το συνδυασμό συντηρητικής και χειρουργικής αντιμετώπισης.27
Ο τύπος Ι συγγενούς ΚΟΤ μπορεί να αντιμετωπιστεί τόσο συντηρητικά όσο και χειρουργικά με πολύ καλά αποτελέσματα.11,12,14-16,22 Υπάρχει διχογνωμία όμως μεταξύ των χειρουργών σχετικά με την απόφαση για χειρουργική ή συντηρητική αντιμετώπιση. Μερικοί χειρουργοί προτείνουν άμεση χειρουργική αντιμετώπιση στη φυλή sharpei αφού τα περισσότερα ζώα της φυλής αυτής φαίνεται να μην ανταποκρίνονται στη συντηρητική αγωγή.15,22,47 Η αντιμετώπιση πάντως της πρωτογενούς αιτίας συμβάλει στην υποχώρηση των συμπτωμάτων.2,41,42 Η συντηρητική αγωγή γενικότερα στοχεύει στην αντιμετώπιση των συμπτωμάτων της οισοφαγίτιδας από ΓΟΠ. Ειδικότερα οι στόχοι της συντηρητικής αγωγής περιλαμβάνουν την ελάττωση του όγκου του υγρού της παλινδρόμησης, της έκκρισης και την αύξηση του pH του γαστρικού υγρού, την προστασία του οισοφαγικού βλεννογόνου από την δράση του παλινδρομούντος υγρού και την επιτάχυνση της γαστρικής κένωσης με τη σύγχρονη αύξηση του τόνου του οπίσθιου οισοφαγικού σφικτήρα.2,12,16 Αυτό επιτυγχάνεται με τη χορήγηση δίαιτας με χαμηλά λιπαρά σε συχνά γεύματα, τη χορήγηση Η2 αναστολέων ή αναστολέων της αντλίας πρωτονίων, γαστροπροστατευτικών και γαστροκινητικών. Σε περίπτωση μεγαοισοφάγου η χορήγηση τροφής θα πρέπει να γίνεται από ύψος. Οι δραστικές ουσίες που χρησιμοποιούνται για τη συντηρητική αγωγή της ΚΟΤ και η δοσολογία τους περιγράφονται στον πίνακα 2. Η συντηρητική αγωγή διαρκεί 30 ημέρες και μόνο σε περίπτωση που τα αποτελέσματά της είναι πτωχά συνιστάται η χειρουργική αντιμετώπιση. Η απόφαση πάντως για το ποια αγωγή θα δοθεί στη συνέχεια πρέπει να λαμβάνεται σε εξατομικευμένη βάση.3,12,16 Σύμφωνα με μια μελέτη 8 από τους 15 σκύλους και γάτες με συγγενή ΚΟΤ τύπου Ι που αντιμετωπίστηκαν συντηρητικά εμφάνισαν ίαση.16 Στα ζώα που δεν έχουν κλινική συμπτωματολογία δεν απαιτείται καμία θεραπεία.12 Στην κήλη τύπου ΙΙ δεν παρατηρείται ΓΟΠ αφού ο οπίσθιος οισοφαγικός σφικτήρας παραμένει στη θέση του. Στον τύπο αυτό η συμπτωματολογία οφείλεται στη πρόπτωση του στομάχου ή άλλων σπλάχνων στην θωρακική κοιλότητα και επομένως απαιτείται πάντοτε χειρουργική θεραπεία.25,26,28 Η παρουσία όμως μεγαοισοφάγου και κατά συνέπεια ΓΟΠ αποτελεί εξαίρεση και επιβάλει το συνδυασμό συντηρητικής και χειρουργικής αντιμετώπισης.27
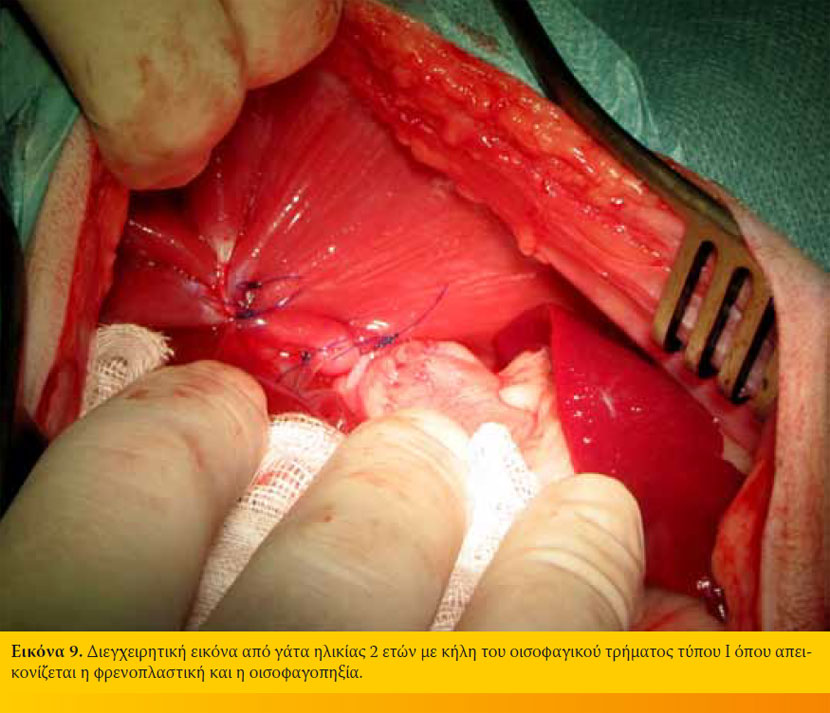
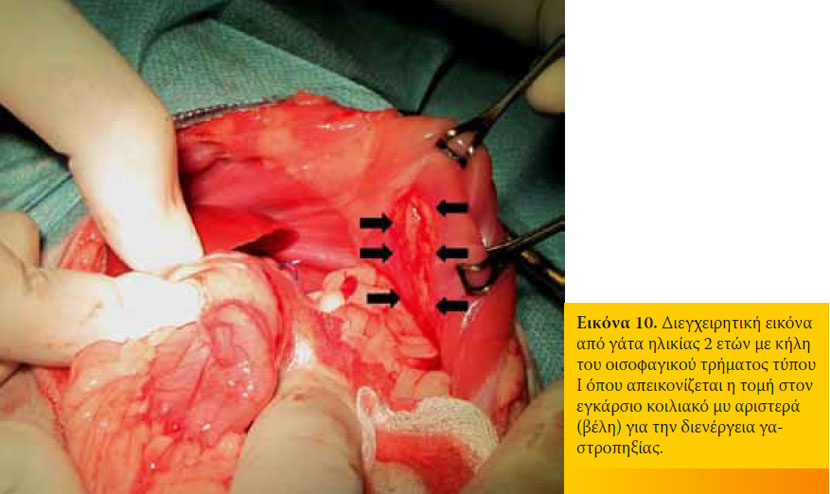
Χειρουργική αγωγή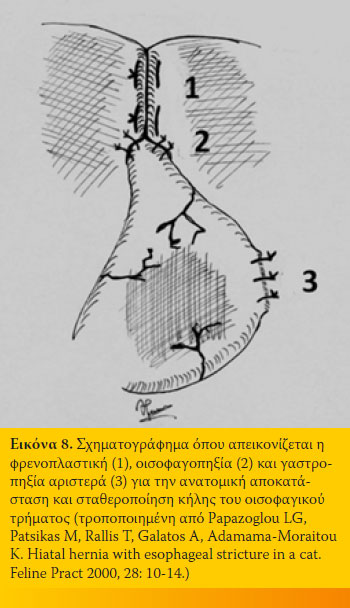 Η χειρουργική αντιμετώπιση της ΚΟΤ ενδείκνυται σε αποτυχία της συντηρητικής αγωγής, μετά το πέρας των 30 ημερών που διαρκεί αυτή, σε κήλες τύπου II-IV και σε σκύλους της φυλής sharpei. 12,15,16,22,47 Παλαιότερα η χειρουργική αντιμετώπιση της ΚΟΤ είχε ως σκοπό την ενίσχυση του οπίσθιου οισοφαγικού σφικτήρα, που θεωρούνταν ότι είχε ανεπάρκεια ή αχαλασία, με τη χρήση διάφορων θολοπλαστικών τεχνικών. Οι τεχνικές αυτές χαρακτηρίζονταν από υψηλό ποσοστό επιπλοκών και εγκαταλείφθηκαν αφού η θεωρία της αχαλασίας καταρρίφθηκε.6,10-12,16 Η ανατομική αποκατάσταση και σταθεροποίηση της ΚΟΤ αποτελεί τη χειρουργική θεραπεία εκλογής στην εποχή μας.11 Η επέμβαση αυτή εγγυάται τα καλύτερα αποτελέσματα με την απλούστερη εγχειρητική τεχνική. Η επέμβαση σκοπεύει στην ελάττωση της διαμέτρου του οισοφαγικού τρήματος (φρενοπλαστική), στην καθήλωση του οισοφάγου στο διαφραγματικό σκέλος με οισοφαγοπηξία και στην καθήλωση του στομάχου στο αριστερό κοιλιακό τοίχωμα με γαστροπηξία (Εικόνα 8).11 Σε περίπτωση ύπαρξης εισροφητικής βρογχοπνευμονίας συστήνεται προεγχειρητικά η χορήγηση της κατάλληλης αντιβιοθεραπείας. Η προσπέλαση του οισοφαγικού τρήματος γίνεται διαμέσου μέσης λαπαροτομής και αφού προηγηθεί καθετηριασμός του οισοφάγου για την ευκολότερη αναγνώρισή του : διατέμνεται ο ηπατογαστρικός σύνδεσμος οι αριστεροί λοβοί του ήπατος φέρονται προς τα έσω και ο στόμαχος προς τα δεξιά. Ο φρενοοισοφαγικός σύνδεσμος διατέμνεται κυκλοτερώς, απελευθερώνεται ο οισοφάγος και έλκεται προς την κοιλιακή κοιλότητα, λαμβάνοντας μέριμνα για την αποφυγή τραυματισμού των κοιλιακών κλάδων του πνευμονογαστρικού νεύρου. Με το χειρισμό αυτόν όμως προκαλείται πνευμοθώρακας και απαιτείται τεχνητός αερισμός με θετική πίεση και εκκένωση της θωρακικής κοιλότητας. Η φρενοπλαστική γίνεται σε μήκος 1-2 cm, με τη μερική συμπλησίαση των σκελών του διαφράγματος, κοιλιακά του οισοφάγου, με απλές χωριστές ή οριζόντια επιστρεφόμενες ραφές, με μη απορροφήσιμο μονόκλωνο ράμμα.11,14 Στο τέλος της συρραφής το ένα ή τα δύο δάκτυλα του χειρουργού θα πρέπει να μπορούν να εισέλθουν στο τρήμα κατά μήκος του οισοφάγου χωρίς να προκαλείται στένωσή του.10 Με την τεχνική αυτή ο οπίσθιος οισοφαγικός σφικτήρας μετακινείται ραχιαία. Μερικοί χειρουργοί υποστηρίζουν τη διενέργεια φρενοπλαστικής, χωρίς τη διατομή του φρενοοισοφαγικού συνδέσμου, με τη τοποθέτηση οριζόντια επιστρεφόμενων ραφών, τόσο κοιλιακά όσο και ραχιαία, διαμέσου των διαφραγματικών σκελών.22 Η οισοφαγοπηξία επιτυγχάνεται με την τοποθέτηση μερικών απλών χωριστών ραφών μεταξύ του οισοφάγου και του διαφράγματος αριστερά ή με τη διενέργεια δύο τομών μήκους 3 cm στο μυϊκό χιτώνα του οισοφάγου και στο διάφραγμα και τη μεταξύ τους συρραφή με ράμμα (Εικόνα 9). Η επέμβαση ολοκληρώνεται με τη γαστροπηξία του γαστρικού θόλου στο αριστερό κοιλιακό τοίχωμα που γίνεται με τομή ή με τοποθέτηση σωλήνα γαστροστομίας έτσι ώστε να παρεμποδίζεται η πρόσθια μετατόπιση του στομάχου (Εικόνα 10). Με την γαστροπηξία στη θέση αυτή επιτυγχάνεται αύξηση της πίεσης του οπίσθιου οισοφαγικού σφικτήρα και κατά συνέπεια παρεμπόδιση της ΓΟΠ.38 Η μετεγχειρητική πρόγνωση χαρακτηρίζεται από πολύ καλή έως άριστη. 11,15,16,22
Η χειρουργική αντιμετώπιση της ΚΟΤ ενδείκνυται σε αποτυχία της συντηρητικής αγωγής, μετά το πέρας των 30 ημερών που διαρκεί αυτή, σε κήλες τύπου II-IV και σε σκύλους της φυλής sharpei. 12,15,16,22,47 Παλαιότερα η χειρουργική αντιμετώπιση της ΚΟΤ είχε ως σκοπό την ενίσχυση του οπίσθιου οισοφαγικού σφικτήρα, που θεωρούνταν ότι είχε ανεπάρκεια ή αχαλασία, με τη χρήση διάφορων θολοπλαστικών τεχνικών. Οι τεχνικές αυτές χαρακτηρίζονταν από υψηλό ποσοστό επιπλοκών και εγκαταλείφθηκαν αφού η θεωρία της αχαλασίας καταρρίφθηκε.6,10-12,16 Η ανατομική αποκατάσταση και σταθεροποίηση της ΚΟΤ αποτελεί τη χειρουργική θεραπεία εκλογής στην εποχή μας.11 Η επέμβαση αυτή εγγυάται τα καλύτερα αποτελέσματα με την απλούστερη εγχειρητική τεχνική. Η επέμβαση σκοπεύει στην ελάττωση της διαμέτρου του οισοφαγικού τρήματος (φρενοπλαστική), στην καθήλωση του οισοφάγου στο διαφραγματικό σκέλος με οισοφαγοπηξία και στην καθήλωση του στομάχου στο αριστερό κοιλιακό τοίχωμα με γαστροπηξία (Εικόνα 8).11 Σε περίπτωση ύπαρξης εισροφητικής βρογχοπνευμονίας συστήνεται προεγχειρητικά η χορήγηση της κατάλληλης αντιβιοθεραπείας. Η προσπέλαση του οισοφαγικού τρήματος γίνεται διαμέσου μέσης λαπαροτομής και αφού προηγηθεί καθετηριασμός του οισοφάγου για την ευκολότερη αναγνώρισή του : διατέμνεται ο ηπατογαστρικός σύνδεσμος οι αριστεροί λοβοί του ήπατος φέρονται προς τα έσω και ο στόμαχος προς τα δεξιά. Ο φρενοοισοφαγικός σύνδεσμος διατέμνεται κυκλοτερώς, απελευθερώνεται ο οισοφάγος και έλκεται προς την κοιλιακή κοιλότητα, λαμβάνοντας μέριμνα για την αποφυγή τραυματισμού των κοιλιακών κλάδων του πνευμονογαστρικού νεύρου. Με το χειρισμό αυτόν όμως προκαλείται πνευμοθώρακας και απαιτείται τεχνητός αερισμός με θετική πίεση και εκκένωση της θωρακικής κοιλότητας. Η φρενοπλαστική γίνεται σε μήκος 1-2 cm, με τη μερική συμπλησίαση των σκελών του διαφράγματος, κοιλιακά του οισοφάγου, με απλές χωριστές ή οριζόντια επιστρεφόμενες ραφές, με μη απορροφήσιμο μονόκλωνο ράμμα.11,14 Στο τέλος της συρραφής το ένα ή τα δύο δάκτυλα του χειρουργού θα πρέπει να μπορούν να εισέλθουν στο τρήμα κατά μήκος του οισοφάγου χωρίς να προκαλείται στένωσή του.10 Με την τεχνική αυτή ο οπίσθιος οισοφαγικός σφικτήρας μετακινείται ραχιαία. Μερικοί χειρουργοί υποστηρίζουν τη διενέργεια φρενοπλαστικής, χωρίς τη διατομή του φρενοοισοφαγικού συνδέσμου, με τη τοποθέτηση οριζόντια επιστρεφόμενων ραφών, τόσο κοιλιακά όσο και ραχιαία, διαμέσου των διαφραγματικών σκελών.22 Η οισοφαγοπηξία επιτυγχάνεται με την τοποθέτηση μερικών απλών χωριστών ραφών μεταξύ του οισοφάγου και του διαφράγματος αριστερά ή με τη διενέργεια δύο τομών μήκους 3 cm στο μυϊκό χιτώνα του οισοφάγου και στο διάφραγμα και τη μεταξύ τους συρραφή με ράμμα (Εικόνα 9). Η επέμβαση ολοκληρώνεται με τη γαστροπηξία του γαστρικού θόλου στο αριστερό κοιλιακό τοίχωμα που γίνεται με τομή ή με τοποθέτηση σωλήνα γαστροστομίας έτσι ώστε να παρεμποδίζεται η πρόσθια μετατόπιση του στομάχου (Εικόνα 10). Με την γαστροπηξία στη θέση αυτή επιτυγχάνεται αύξηση της πίεσης του οπίσθιου οισοφαγικού σφικτήρα και κατά συνέπεια παρεμπόδιση της ΓΟΠ.38 Η μετεγχειρητική πρόγνωση χαρακτηρίζεται από πολύ καλή έως άριστη. 11,15,16,22
> Βιβλιογραφία
1. Hunt JB. Hiatal hernia. In: Mechanisms of Disease in Small Animal Surgery. Bojrab MJ, Monnet E (eds). 3rd edn. Teton New Media: Jackson, 2010, pp. 138-141.
2. Bright R. Hiatal hernia. In: Small Animal Soft Tissue Surgery. Monnet E(ed). 1st edn.Wiley- Blackwell: Ames, 2013, pp. 321-327.
3. Sivacolundhu RK, Read RA, Marchevsky AM. Hiatal hernia controversies – a review of pathophysiology and treatment options. Aust Vet J 2002, 80: 48-53.
4. Gordon LC, Friend EA, Hamilton MH. Hemorrhagic pleural effusion secondary to an unusual type III hiatal hernia in a 4-year-old Great Dane. J Am Anim Hosp Assoc 2010, 46: 336-340.
5. Cornell K. Stomach. In: Veterinary Surgery Small Animals. Tobias KM, Johnston SA (eds). 1st edn. Elsevier Saunders: St Louis, 2012, pp. 1500-1512.
6. Gaskell CJ, Gibbs C, Pearson H. Sliding hiatus hernia with reflux oesophagitis in two dogs. J Small Anim Pract 1974, 15: 503-509.
7. Robotham GR. Congenital hiatal hernia in a cat. Feline Pract 1979, 9: 37-39.
8. Dhein CRM, Rawlings CA, Rosin E, Losonsky JM, Chambers JN. Esophageal hiatal hernia and eventration of the diaphragm with resultant gastroesophageal reflux. J Am Anim Hosp Assoc 1980, 16: 517-522.
9. Peterson SL. Esophageal hiatal hernia in a cat. J Am Vet Med Assoc 1983, 183: 325-326.
10. Ellison GW, Lewis DD, Phillips L, Tarvin GB. Esophageal hiatal hernia in small animals: literature review and a modified surgical technique. J Am Anim Hosp Assoc 1986, 23: 391-399.
11. Prymak C, Saunders HM, Washabau RJ. Hiatal hernia repair by restoration and stabilization of normal anatomy an evaluation in four dogs and one cat. Vet Surg 1989, 18: 386-391.
12. Bright RM, Sackman JE, DeNovo C, Toal C. Hiatal hernia in the dog and cat: a retrospective study of 16 cases. J Small Anim Pract 1990, 31: 244-250.
13. Waldron DR, Moon M, Leib MS, Barber D, Mays KA. Oesophageal hiatal hernia in two cats. J Small Anim Pract 1990, 31: 259-263.
14. White RN. A modified technique for surgical repair of oesophageal hiatal herniation in the dog. J Small Anim Pract 1993, 34: 599-603.
15. Callan MB, Washabau RJ, Saunders HM, Kerr L, Prymak C, Holt D. Congenital esophageal hiatal hernia in the Chinese Shar-Pei dog. J Vet Intern Med 1993, 7: 210-215.
16. Lorinson D, Bright RM. Long-term outcome of medical and surgical treatment of hiatal hernias in dogs and cats: 27 cases (1978-1996). J Am Vet Med Assoc 1998, 213: 381-384.
17. Pratschke KM, Hughes JML, Skelly C, Bellenger CR. Hiatal herniation as a complication of chronic diaphragmatic herniation. J Small Anim Pract 1998, 39: 33-38.
18. Hardie EM, Ramirez O, Clary EM, Kornegay JN, Correa MT, Feimster RA, Robertson ER. Abnormalities of the thoracic bellows: stress fractures of the ribs and hiatal hernia. J Vet Intern Med 1998, 12: 279-287.
19. Papazoglou LG, Patsikas M, Rallis T, Galatos A, Adamama-Moraitou K. Hiatal hernia with esophageal stricture in a cat. Feline Pract 2000, 28: 10-14.
20. Hunt GB, O’Brien C, Kolenc G, Malik R. 2002 : hiatal hernia in a puppy. Aust Vet J 2002, 80: 685-686.
21. Owen MC, Morris PJ, Bateman RS. Concurrent gastro-oesophageal intussusception, trichobezoar and hiatal hernia in a cat. N Z Vet J 2005, 53: 371-374.
22. Guiot LP, Lansdowne JL, Rouppert P, Stanley BJ. Hiatal hernia in the dog: a clinical report of four Chinese Shar Peis. J Am Anim Hosp Assoc 2008, 44: 335-341.
23. Keeley B, Puggioni A, Pratschke K. Congenital oesophageal hiatal hernia in a pug. Irish Vet J 2008, 61: 389-393.
24. DeSandre-Robinson DM, Madden SN, Walker JT. Nasopharyngeal stenosis with concurrent hiatal hernia and megaesophagus in an 8-year-old cat. J Feline Med Surg 2011, 13: 454-459.
25. Teunissen GHB, Happe RP, Van Toorenburg J, Wolvekamp WTHC. Esophageal hiatal hernia case report of a dog and a cheetah. Tijdschr Diergeneeskd 1978, 103: 742-749.
26. Miles KG, Pope ER, Jergens AE. Paraesophageal hiatal hernia and pyloric obstruction in a dog. J Am Vet Med Assoc 1988, 193: 1437-1439.
27. Kirkby KA, Bright RM, Owen HD. Paraoesophageal hiatal hernia and megaoesophagus in a three-week-old Alaskan malamute. J Small Anim Pract 2005, 46: 402-405.
28. Mitsuoka K, Tanaka R, Nagashima Y, Hoshi K, Matsumoto H, Yamane Y. Omental herniation through the esophageal hiatus in a cat. J Vet Med Sci 2002, 64: 1157-1159.
29. Williams JM. Hiatal hernia in a Shar-Pei. J Small Anim Pract 1990, 31: 251-254.
30. Auger JM, Riley SM. Combined hiatal and pleuroperitoneal hernia in a Shar-Pei. Can Vet J 1997, 38: 640-642.
31. Baig MA, Gemmill T, Hammond G, Patterson C, Ramsey IK. Budd-chiari-like syndrome caused by a congenital hiatal hernia in a Shar-Pei dog. Vet Rec 2006, 159: 322-323.
32. Rahal SC, Mamprim MJ, Muniz LMR, Teixeira CR. Type-4 esophageal hiatal hernia in a Chinese Shar-Pei dog. Vet Radiol Ultrasound 2003, 44: 646-647.
33. Bremner CG, Shorter RG, Ellis FH. Anatomy of feline esophagus with special reference to its muscular wall and phrenoesophageal membrane. J Surg Res 1970, 10: 327-331.
34. Botha GSM. A note on the comparative anatomy of the cardio-esophageal junction. Acta Anat (Basel) 1958, 34: 52-58.
35. Clark CG, Vane JR. The cardiac sphincter in the cat. Gut 1961, 2: 252-262.
36. Pratschke KM, Fitzpatrick E, Campion D, McAllister H, Bellenger CR. Topography of the gastro-oesophageal junction in the dog revisited: possible clinical implications. Res Vet Sci 2004, 76: 171-177.
37. Alsafy MAM, El-Gendy SAA. Gastroesophageal junction of Anatolian shepherd dog; a study by topographic anatomy, scanning electron and light microscopy. Vet Res Commun 2012, 36:63-69.
38. Pratschke KM, Bellenger CR, McAllister H, Campion D. Barrier pressure at the gastroesophageal junction in anesthetized dogs. Am J Vet Res 2001, 62: 1068-1072.
39. Han E. Diagnosis and management of reflux esophagitis. Clin Tech Small Anim Pract 2003, 18: 231- 238.
40. Stickle R, Sparschu G, Love N, Walshaw R. Radiographic evaluation of esophageal function in Chinese Shar Pei pups. J Am Vet Med Assoc 1992, 201: 81-84.
41. Poncet CM, Dupre GP, Freiche VG, Estrada MM, Poubanne YA, Bouvy BM. Prevalence of gastrointestinal tract lesions in 73 brachycephalic dogs with upper respiratory syndrome. J Small Anim Pract 2005, 46: 273- 279.
42. Poncet CM, Dupre GP, Freiche VG, Bouvy BM. Longterm results of upper respiratory syndrome surgery and gastrointestinal tract medical treatment in 51 brachycephalic dogs. J Small Anim Pract 2006, 47: 137- 142.
43. Barnie AG, Simpson JW, Corcoran BM. Gastrooesophageal reflux and hiatus hernia associated with laryngeal paralysis in a dog. J Small Anim Pract 1989, 30: 414-416.
44. Dvir E, Spotswood TC, Lambrechts NE, Lobetti RG. Congenital narrowing of the intrapharyngeal opening in a dog with concurrent oesophageal hiatal hernia. J Small Anim Pract 2003, 44: 359-362.
45. Dieringer TM, Wolf AM. Esophageal hiatal hernia and megaesophagus complicating tetanus in two dogs. J Am Vet Med Assoc 1991, 199: 87-89.
46. Van Ham L, Van Bree H. Conservative treatment of tetanus associated with hiatus hernia and gastrooesophageal reflux. J Small Anim Pract 1992, 33: 289- 294.
47. Holt D, Callan MB, Washabau RJ, Saunders MH. Medical treatment versus surgery for hiatal hernias. J Am Vet Med Assoc 1998, 213: 800.




