Παθογένεια, διάγνωση και σύγχρονες θεραπευτικές επιλογές
> Περίληψη
Η δυσπλασία του αγκώνα είναι μία νόσος, η οποία προκαλεί πόνο και χωλότητα σε σκύλους μεγαλόσωμων και γιγαντόσωμων φυλών. Οφείλεται σε γενετικούς παράγοντες, οι οποίοι σε συνδυασμό με περιβαλλοντικούς παράγοντες, διαταράσσουν την ανάπτυξη της άρθρωσης του αγκώνα. Παλιότερα, ως κύρια αιτιολογία πρόκλησης της νόσου θεωρούνταν η οστεοχονδρίτιδα του αγκώνα. Από σύγχρονες όμως μελέτες υποστηρίζεται ότι η νόσος, οφείλεται, τις περισσότερες φορές, στις ποικίλες μορφές δυσαρμονίας μεταξύ των αρθρικών επιφανειών των τριών αρθρώσεων που σχηματίζουν την άρθρωση του αγκώνα. Η θεραπεία της είναι χειρουργική και πρέπει να εφαρμόζεται πριν από την εμφάνιση στην άρθρωση αλλοιώσεων οστεοαρθρίτιδας. Βιβλιογραφικά περιγράφονται διάφορες χειρουργικές τεχνικές αντιμετώπισης της νόσου. Σε περιπτώσεις που στην ακτινολογική εξέταση της άρθρωσης του αγκώνα απεικονίζονται βαριές αλλοιώσεις οστεοαρθρίτιδας, η επιλογή της χειρουργικής τεχνικής εξαρτάται από την κατανομή των αλλοιώσεων.
> Εισαγωγή
Η δυσπλασία του αγκώνα είναι κληρονομική νόσος, η οποία χαρακτηρίζεται από τη μη φυσιολογική ανάπτυξη της άρθρωσης του αγκώνα. Από το 1993 η Διεθνής Ομάδα Εργασίας για τον Αγκώνα (International Elbow Working Group, IEWG) όρισε, ότι οι κληρονομικές παθολογικές καταστάσεις που προσβάλλουν την άρθρωση του αγκώνα και αναφέρονται συνοπτικά με τον όρο «δυσπλασία του αγκώνα», είναι η αδυναμία συνοστέωσης του ράμφους του ωλεκράνου (ΑΣΡΩ), η διαχωριστική οστεοχονδρίτιδα της τροχιλίας του βραχιόνιου οστού (ΔΟ), η νόσος της έσω κορωνοειδούς απόφυσης της ωλένης (NEKA) και η δυσαρμονία μεταξύ των αρθρικών επιφανειών των οστών τα οποία απαρτίζουν τις διαρθρώσεις της άρθρωσης του αγκώνα (ΔΑ).1
Η νόσος προσβάλλει κυρίως σκύλους μεγαλόσωμων και γιγαντόσωμων φυλών. Συχνότερα προσβάλλονται οι φυλές Bernese Mountain dog,2 Labrador retriever,3 Golden retriever, Rottweiler και German shepherd dog,4 ενώ οι ταχέως αναπτυσσόμενοι αρσενικοί σκύλοι προσβάλλονται σε διπλάσια συχνότητα σε σύγκριση με τους θηλυκούς.5,6 Με μικρότερη συχνότητα είναι δυνατό να προσβάλει και σκύλους μεσαίου μεγέθους, χονδροδυστροφικών φυλών (Dachshund, French bulldog).4
Το κύριο σύμπτωμα του νοσήματος είναι η χωλότητα, η οποία μπορεί να εμφανιστεί από την ηλικία των 3-10 μηνών. Μερικοί σκύλοι εμφανίζουν χωλότητα μετά την ενηλικίωση (>6 ετών), λόγω ΝΕΚΑ, χωρίς να προϋπάρχει ιστορικό χωλότητας σε νεαρότερη ηλικία.7 Σε ποσοστό 37-50% των περιστατικών προσβάλλονται και τα δύο πρόσθια άκρα.8
Επειδή η ΝΕΚΑ, η ΔΟ και η ΔΑ προκαλούν αλλοιώσεις στα ανατομικά στοιχεία του εσωτερικού τμήματος της άρθρωσης του αγκώνα (έσω κορωνοειδής απόφυση της ωλένης, τροχιλιακή εντομή της ωλένης και τροχιλία του βραχιόνιου), και επιπλέον, επειδή οι τρεις αυτές παθολογικές καταστάσεις μπορεί να συνυπάρχουν στην άρθρωση, προτάθηκε να χρησιμοποιείται αντί των όρων αυτών, ο γενικότερος όρος «νόσος του εσωτερικού τμήματος της άρθρωσης του αγκώνα» (ΝΕΤΑ).9
> Παθογένεια
Η γενετική βάση της δυσπλασίας του αγκώνα έχει διερευνηθεί με αρκετές και μεγάλες επιδημιολογικές μελέτες. Βάση αυτών φαίνεται ότι η νόσος κληρονομείται με διαφορετικό τρόπο σε κάθε φυλή σκύλων. Επίσης, υπάρχει η σοβαρή υπόθεση, ότι κάθε μορφή δυσπλασίας του αγκώνα κληρονομείται ανεξάρτητα από την άλλη. Το συμπέρασμα είναι, ότι η δυσπλασία του αγκώνα οφείλεται σε διαφορετικές γενετικές νόσους, οι οποίες διαταράσσουν την ανάπτυξη της άρθρωσης του αγκώνα με διαφορετικούς μηχανισμούς. Λόγω της πολυπλοκότητας της κληρονομικής μεταβίβασης και της επίδρασης των περιβαλλοντολογικών παραγόντων στην εκδήλωση της νόσου, υποστηρίζεται ότι είναι αδύνατος ο γενετικός έλεγχος της δυσπλασίας του αγκώνα στο άμεσο μέλλον.10,11,12
Αναφέρονται τρεις αιτιολογικοί μηχανισμοί που εμπλέκονται στην πρόκληση της δυσπλασίας του αγκώνα. Η οστεοχόνδρωση,13,14 η δυσαρμονία μεταξύ των αρθρικών επιφανειών των οστών των επιμέρους διαρθρώσεων της άρθρωσης του αγκώνα15 και η στροφική αστάθεια της κερκιδωλενικής διάρθρωσης.16,17
Οι αιτιολογικοί μηχανισμοί, οι οποίοι είναι αποτέλεσμα γενετικής προδιάθεσης, σε συνδυασμό με δευτερογενείς προδιαθέτοντες παράγοντες, όπως είναι η υψηλοθερμιδική διατροφή και η υπερβολική άσκηση, αποτελούν τα κύρια αίτια κλινικής εκδήλωσης της νόσου.9
Σε σύγχρονες μελέτες υποστηρίζεται, ότι από τους τρεις αιτιολογικούς μηχανισμούς ο πιο πιθανός για την πρόκληση της νόσου είναι η δυσαρμονία μεταξύ των αρθρικών επιφανειών των οστών των επιμέρους διαρθρώσεων της άρθρωσης του αγκώνα. Σε μερικούς σκύλους η οστεοχόνδρωση παίζει σημαντικό αιτιολογικό ρόλο. Ο μηχανισμός της στροφικής αστάθειας της κερκιδωλενικής διάρθρωσης βρίσκεται υπό έρευνα.
Α. Οστεοχόνδρωση
Σύμφωνα με την κλασική θεωρία, η οστεοχόνδρωση είναι υπεύθυνη για τις αλλοιώσεις στην έσω κορωνοειδή απόφυση, στην τροχιλία του βραχιόνιου οστού και στο συζευκτικό χόνδρο του ράμφους του ωλεκράνου.13,18
Φυσιολογικά, η χόνδρινη έσω κορωνοειδής απόφυση οστεοποιείται από τη βάση προς τη κορυφή της. Έχει αποδειχθεί ότι στερείται ξεχωριστού πυρήνα οστέωσης, αλλά έχει τον ίδιο πυρήνα οστέωσης με το κεντρικό τμήμα της ωλένης. Η διαδικασία της οστεοποίησης ολοκληρώνεται στην ηλικία των 5-5½ μηνών. Εάν διαταραχθεί η ενδοχόνδρια οστέωση της χόνδρινης έσω κορωνοειδούς απόφυσης προκαλείται θάνατος των βαθύτερων κυττάρων του χόνδρου, με αποτέλεσμα τη χονδρομαλακία και τη δημιουργία ρωγμών. Τα τμήματα αυτά, της έσω κορωνοειδούς απόφυσης συνήθως ασβεστοποιούνται, επειδή διαταράσσεται η αιμάτωσή τους, η οποία γίνεται διαμέσου της ινώδους σύνδεσής τους με το δακτυλιοειδή σύνδεσμο.
Η θεωρία αυτή βρίσκεται σε αντίθεση με τα υποστηριζόμενα σε μία πιο σύγχρονη μελέτη, η οποία βασίστηκε σε ιστοπαθολογικές εξετάσεις της κορωνοειδούς απόφυσης σε κλινικά περιστατικά.19 Σύμφωνα με αυτή, δεν διαπιστώθηκαν αλλοιώσεις οστεοχόνδρωσης στα προσβεβλημένα τμήματα της έσω κορωνοειδούς απόφυσης, αλλά αλλοιώσεις όμοιες με αυτές που παρατηρούνται στα κατάγματα. Συμπεραίνεται, ότι οι αλλοιώσεις αυτές οφείλονται στη μεγάλη και συνεχή φόρτιση της χόνδρινης έσω κορωνοειδούς απόφυσης και τη δημιουργία καταγμάτων λόγω κόπωσης, με συνέπεια την αδυναμία πώρωσης του ινώδη ιστού της.
Β. Δυσαρμονία μεταξύ των αρθρικών επιφανειών των επιμέρους διαρθρώσεων της άρθρωσης του αγκώνα.
Η άρθρωση του αγκώνα είναι μία σύνθετη διάρθρωση αποτελούμενη από τρεις επιμέρους διαρθρώσεις, οι οποίες είναι η βραχιονιοκερκιδική (οι αρθρικές επιφάνειες είναι ο κόνδυλος του βραχιόνιου και η κεφαλή της κερκίδας), η βραχιονιωλενική (οι αρθρικές επιφάνειες είναι η τροχιλία του βραχιόνιου, που συντάσσεται με τη τροχιλιακή ή μηνοειδή εντομή και την έσω κορωνεοειδή απόφυση της ωλένης) και η κερκιδωλενική διάρθρωση (οι αρθρικές επιφάνειες είναι η οπίσθια αρθρική επιφάνεια της κερκίδας και η κερκιδική εντομή της ωλένης).19
Έχουν διαπιστωθεί ως μορφές δυσαρμονίας η διαφορά μήκους μεταξύ κερκίδας και ωλένης, καθώς και η βραχιονιωλενική δυσαρμονία.
Β1. Διαφορά μήκους μεταξύ κερκίδας και ωλένης
Οφείλεται σε ασύγχρονη κατά μήκος αύξηση των δύο οστών. Αναφέρονται δύο παραλλαγές. Στη πρώτη, η κερκίδα είναι βραχύτερη από την ωλένη ή το κεντρικό άκρο της βρίσκεται περιφερικά του επιπέδου της έσω κορωνοειδούς απόφυσης της ωλένης (σύνδρομο βραχείας κερκίδας).15,20 Στη δεύτερη παραλλαγή, η ωλένη είναι βραχύτερη της κερκίδας ή το κεντρικό άκρο της κερκίδας βρίσκεται κεντρικά του επιπέδου της έσω κορωνοειδούς απόφυσης της ωλένης (σύνδρομο βραχείας ωλένης).21
Στο σύνδρομο της βραχείας κερκίδας, ολόκληρη η δύναμη του βάρους του σώματος μεταφέρεται από την τροχιλία του βραχιόνιου στην έσω κορωνοειδή απόφυση της ωλένης. Η έντονη μηχανική φόρτιση, προκαλεί βλάβη λόγω πίεσης στο υποχόνδριο οστό της έσω κορωνοειδούς απόφυσης, με αποτέλεσμα τη δημιουργία σε αυτή ρωγμών ή κατάγματος (εικόνα 1).21

Κατά τη δεύτερη παραλλαγή, η κεφαλή της κερκίδας ασκεί ένα κεντρικά κατευθυνόμενο φορτίο στον κόνδυλο του βραχιόνιου οστού, που στη συνέχεια μεταφέρεται στο ράμφος του ωλεκράνου, εμποδίζοντας τη συνοστέωσή του με τη μετάφυση της ωλένης.22,23
Σύμφωνα με τα παραπάνω και με βάση τη δράση γραμμικών δυνάμεων στην άρθρωση, μπορεί να ερμηνευτούν η ΝΕΚΑ και η ΑΣΡΩ. Με τη θεωρία των γραμμικών δυνάμεων όμως, δεν μπορεί να ερμηνευθεί η συνύπαρξη ΝΕΚΑ και ΑΣΡΩ σε κλινικά περιστατικά.5
Για την ερμηνεία της συνύπαρξης αυτών των παθολογικών καταστάσεων προτάθηκε μια νέα θεωρία, η οποία βασίζεται στη δράση στροφικών δυνάμεων (θεωρία στροφικών δυνάμεων).24 Σύμφωνα με αυτή υφίστανται πάλι δύο παραλλαγές, σχετικά με τη διαφορά μήκους μεταξύ κερκίδας και ωλένης. Στο σύνδρομο της βραχείας κερκίδας, το οποίο παρατηρείται σπανιότερα, η θεωρία των γραμμικών δυνάμεων και η θεωρία των στροφικών δυνάμεων είναι σχετικά όμοιες. Αντίθετα, στο σύνδρομο της βραχείας ωλένης, το οποίο παρατηρείται συχνότερα, η θεωρία των στροφικών διαφέρει από τη θεωρία των γραμμικών δυνάμεων.
Σύμφωνα με τη θεωρία των στροφικών δυνάμεων, στην περίπτωση που η κερκίδα αυξάνεται κατά μήκος με ρυθμό ταχύτερο από την ωλένη, η κεφαλή της κερκίδας ασκεί μία δύναμη με φορά κεντρική προς τον κόνδυλο του βραχιόνιου οστού. Αρχικά, η μετακίνηση του βραχιόνιου οστού κεντρικά, εμποδίζεται από το ράμφος του ωλεκράνου. Στη συνέχεια, καθώς η κερκίδα συνεχίζει να αυξάνει σε μήκος αυξάνει και η φόρτιση στον κόνδυλο του βραχιόνιου οστού, ο οποίος αρχίζει να στρέφεται προς τα έξω. Καθώς το βραχιόνιο οστό στρέφεται προς τα έξω, η οπίσθια εσωτερική επιφάνεια του κονδύλου του βραχιόνιου οστού πιέζει την εξωτερική επιφάνεια της βάσης του ράμφους του ωλεκράνου. Εάν το γεγονός αυτό συμβεί πριν από την οστέωση του συζευκτικού χόνδρου του ράμφους του ωλεκράνου προκύπτει ΑΣΡΩ. Η συνεχιζόμενη προώθηση του βραχιόνιου οστού κεντρικά, σε συνδυασμό με τη σύγχρονη στροφή του, προκαλεί έντονη φόρτιση και τριβή στο σημείο επαφής της οπίσθιας εσωτερικής επιφάνειας του κονδύλου του βραχιόνιου οστού με την εξωτερική επιφάνεια της κεντρικής μοίρας της τροχιλιακής εντομής της ωλένης. Στο σημείο αυτό δημιουργούνται αλλοιώσεις τριβής στο χόνδρο του κονδύλου του βραχιόνιου οστού, καθώς και στο χόνδρο της τροχιλιακής εντομής της ωλένης. Η συνεχιζόμενη φόρτιση της κεφαλής της κερκίδας στον κόνδυλο του βραχιόνιου οστού, σε συνδυασμό με τη δράση του ράμφους του ωλεκράνου ως υπομόχλιου, έχουν ως αποτέλεσμα τη μετακίνηση της τροχιλίας του βραχιόνιου οστού προς τα κάτω και τη συμπίεση της έσω κορωνοειδούς απόφυσης της ωλένης. Η συμπίεση και η τριβή, προκαλούν αλλοιώσεις στην έσω κορωνοειδή απόφυση, καθώς και στο κεντρικό τμήμα της τροχιλίας του βραχιόνιου οστού.
Τέλος, καθώς η στροφή του βραχιόνιου οστού γίνεται όλο και μεγαλύτερη, και ειδικότερα όταν δεν υφίσταται ΑΣΡΩ, προκαλείται ώθηση της τροχιλίας του βραχιόνιου οστού προς τα εμπρός, με συνέπεια να μετατοπίζεται έξω από την τροχιλιακή εντομή της ωλένης και να προκαλείται υπεξάρθρημα της άρθρωσης του αγκώνα.
Β2. Βραχιονιωλενική δυσαρμονία
Αυτή παρατηρείται όταν η ακτίνα καμπυλότητας της τροχιλιακής εντομής της ωλένης είναι μικρότερη της ακτίνας καμπυλότητας της τροχιλίας του βραχιόνιου οστού ή όταν η τροχιλιακή εντομή της ωλένης έχει σχήμα ελλειπτικό. Η γεωμετρική αυτή δυσαρμονία έχει ως συνέπεια τη μη καλή προσαρμογή της τροχιλίας του βραχιόνιου οστού στην τροχιλιακή εντομή της ωλένης, με αποτέλεσμα την άσκηση μη φυσιολογικών φορτίσεων στην περιοχή της έσω κορωνοειδούς απόφυσης.25,26 Έχει διαπιστωθεί ότι στους σκύλους της φυλής Bernese mountain dog υπάρχει προδιάθεση σχηματισμού ελλειπτικού σχήματος τροχιλιακής εντομής της ωλένης.2
Γ. Στροφική αστάθεια της κερκιδωλενικής διάρθρωσης
Όταν υπάρχει δυσαρμονία μεταξύ της οπίσθιας αρθρικής επιφάνειας της κερκίδας με την κερκιδική εντομής της ωλένης, η έκκεντρη έλξη του δικέφαλου βραχιόνιου και του πρόσθιου βραχιόνιου μυ, προκαλεί κατά την κάμψη της άρθρωσης στροφική κίνηση της ωλένης προς τα έξω σε σχέση με την κερκίδα. Η στροφική κίνηση προκαλεί συμπίεση των δύο αρθρικών επιφανειών και πρόκληση κάκωσης στην έσω κορωνοειδή απόφυση και στην κερκιδική εντομή της ωλένης.27
> Διάγνωση
Η κάθε μορφή δυσπλασίας του αγκώνα μπορεί να εμφανίζεται μόνη της ή συνηθέστερα, σε συνδυασμό και με κάποια άλλη. Ανεξάρτητα από τη μορφή της δυσπλασίας τα κλινικά συμπτώματα πάντοτε είναι όμοια, μη επιτρέποντας έτσι την αναγνώριση της μορφής της μόνο με κλινική εξέταση. Τα συμπτώματα αρχίζουν συνήθως από την ηλικία των 3-10 μηνών.
Κατά την επισκόπηση των σκύλων με δυσπλασία του αγκώνα, διαπιστώνεται δύσκαμπτο βάδισμα μετά από ανάπαυση, ή και χωλότητα μετά από άσκηση. Όταν η νόσος προσβάλλει και τα δύο πρόσθια άκρα, η αναγνώριση της χωλότητας είναι δύσκολη. Στη θέση στάσης το πάσχον άκρο βρίσκεται σε απαγωγή και το αντιβράχιο, μαζί με τον άκρο πόδα, σε στροφή προς τα έξω (υπτιασμός). Η θέση αυτή βοηθά στη μείωση των φορτίσεων που ασκούνται στο εσωτερικό τμήμα της άρθρωσης του αγκώνα.28
Ένα από τα πλέον σταθερά ευρήματα της κλινικής εξέτασης, είναι ο πόνος που εκδηλώνεται κατά την ψηλάφηση, καθώς και κατά την εκτέλεση παθητικών κινήσεων στην άρθρωση του αγκώνα. Ο πόνος εκδηλώνεται στη βαθειά ψηλάφηση της κατάφυσης του δικεφάλου βραχιόνιου μυ στο ωλένιο όγκωμα, το οποίο εντοπίζεται στην εσωτερική επιφάνεια της ωλένης, περιφερικά της έσω κορωνοειδούς απόφυσης.29 Επίσης, πόνος εκδηλώνεται κατά την πλήρη κάμψη της άρθρωσης, σε συνδυασμό με στροφή προς τα έξω του αντιβραχίου.
Η εκδήλωση πόνου κατά την κλινική εξέταση, σε συνδυασμό με απουσία κάποιας άλλης αναγνωρίσιμης αιτίας χωλότητας ή πόνου, αποτελεί σημαντική ένδειξη δυσπλασίας αγκώνα. Σε περίπτωση ΑΣΡΩ μπορεί να παρατηρηθεί ύδραθρος.30 Στην ΝΕΚΑ η παρουσία ύδραρθρου δεν είναι τυπική.
Σε σκύλους με χρόνια νόσο, η οποία συνοδεύεται από δευτερογενή οστεοαρθρίτιδα, διαπιστώνεται μείωση του εύρους των κινήσεων της άρθρωσης, κριγμός, μυϊκή ατροφία και διόγκωση της άρθρωσης του αγκώνα.
Έχουν αναφερθεί περιστατικά ενήλικων σκύλων, οι οποίοι εμφανίζουν ετερόπλευρη ή αμφοτερόπλευρη χωλότητα στα πρόσθια άκρα εξαιτίας ΝΕΚΑ, χωρίς ιστορικό χωλότητας σε νεαρή ηλικία.7
Η διαφορική διάγνωση πρέπει πάντα να περιλαμβάνει όλες τις πιθανές αιτίες πρόκλησης χωλότητας ενός πρόσθιου άκρου, όπως παθολογικές καταστάσεις της άρθρωσης του ώμου, κακώσεις τενόντων, χωλότητες νευρολογικής αιτιολογίας και νεοπλασίες.
Για την οριστική διάγνωση και την αναγνώριση της μορφής της δυσπλασίας είναι απαραίτητος ο απεικονιστικός έλεγχος της άρθρωσης του αγκώνα. Η απεικόνιση μπορεί να γίνει με απλή ακτινογραφία και με αξονική τομογραφία (CT) ή μαγνητική τομογραφία (MRI). Με την απλή ακτινογραφία μπορεί να μην απεικονιστούν πρωτογενή ευρήματα δυσπλασίας. Στις περιπτώσεις αυτές η διάγνωση βασίζεται στην απεικόνιση των δευτερογενών ευρημάτων οστεοαρθρίτιδας, τα οποία που εμφανίζονται μετά την ηλικία των 7 μηνών.
Η απλή ακτινογράφηση δεν έχει καλή διαγνωστική συνεισφορά στη διάγνωση της ΝΕΚΑ. Για παράδειγμα, οι διαβρώσεις στον αρθρικό χόνδρο της τροχιλίας ή οι ρωγμές στο υποχόνδριο οστό της έσω κορωνοειδούς απόφυσης της ωλένης, δεν απεικονίζονται.31,32,33,34
Εάν σε ένα σκύλο με κλινικά συμπτώματα δυσπλασίας αγκώνα δεν απεικονιστούν αλλοιώσεις στην απλή ακτινογραφία ή αυτές είναι ασαφείς, προτείνεται περαιτέρω διερεύνηση με αξονική ή μαγνητική τομογραφία. Με την αξονική τομογραφία απεικονίζονται οι οστικές δομές της άρθρωσης του αγκώνα χωρίς συμπροβολή των οστών.35 Ως εκ τούτου, έχει μεγαλύτερη ειδικότητα και ευαισθησία για τη διάγνωση της ΝΕΚΑ σε σύγκριση με τις απλές ακτινογραφίες (πίνακας 1).8,36
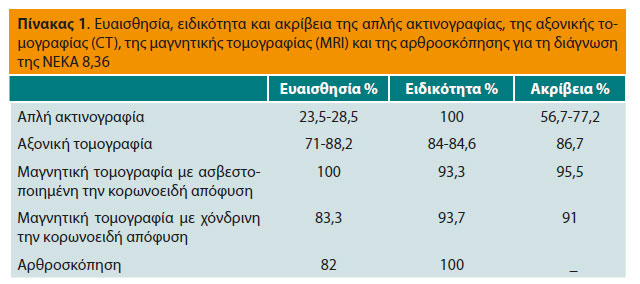
Παρόλα αυτά, είναι δυνατόν στην αξονική και στη μαγνητική τομογραφία να μην απεικονισθούν με σαφήνεια οι αλλοιώσεις στο υποχόνδριο οστό της έσω κορωνοειδούς απόφυσης. Στην περίπτωση που τα ευρήματα όλων των απεικονιστικών εξετάσεων είναι ασαφή συνιστάται η διενέργεια αρθροσκόπησης .
Σε ποσοστό 37-50% των περιστατικών η νόσος προσβάλλει και τα δύο πρόσθια άκρα, οπότε είναι απαραίτητη η απεικονιστική εξέταση και των δύο αρθρώσεων.8
Για την απλή ακτινολογική εξέταση απαιτούνται καλής ποιότητας ακτινογραφίες με το σκύλο τοποθετημένο σε σωστή θέση. Είναι απαραίτητη η χορήγηση ηρέμησης ή γενικής αναισθησίας. Σε όλες τις θέσεις το άκρο τοποθετείται επάνω από την κασέτα χωρίς τη χρήση ακτινοδιαχυτικού πλέγματος. Επίσης, πρέπει να γίνονται ακτινογραφίες στην άρθρωση του ώμου για πιθανή οστεοχονδρίτιδα, που μπορεί να αποτελεί την αιτία της χωλότητας ή να συνυπάρχει με τη δυσπλασία του αγκώνα.
Για να απεικονιστούν όλα τα βασικά ανατομικά στοιχεία της άρθρωσης και όλες οι πιθανές παθολογικές καταστάσεις, πρέπει να λαμβάνονται ακτινογραφίες με το άκρο σε 4 διαφορετικές θέσεις. Οι θέσεις αυτές είναι η πλαγιο-πλάγια με τον αγκώνα σε έκταση, η πλαγιο-πλάγια με τον αγκώνα σε κάμψη, η προσθιο-οπίσθια και η λοξή προσθιοεξωτερική ή οπισθιοεσωτερική ακτινογραφία (150). Στις δύο πρώτες, ο σκύλος τοποθετείται σε πλάγια κατάκλιση και στις άλλες δύο σε στερνική.
Α. Πλαγιο-πλάγια ακτινογράφηση του αγκώνα με την άρθρωση σε έκταση.
Στη θέση αυτή, η γωνία μεταξύ βραχιόνιου οστού και αντιβραχίου πρέπει να είναι περίπου 110ο. Το άκρο τοποθετείται σε τέτοια θέση ώστε να συμπροβάλλονται οι κόνδυλοι του βραχιόνιου οστού.
Η απεικόνιση της φυσιολογικής άρθρωσης του αγκώνα, σε σκύλο ηλικίας μεγαλύτερης των 6 μηνών, χαρακτηρίζεται από αρμονία μεταξύ των αρθρικών επιφανειών και ομοιόμορφα λεπτού εύρους αρθρικά διαστήματα μεταξύ του βραχιόνιου οστού, της κερκίδας και της ωλένης. Επίσης, η ακρολοφία της τροχιλιακής εντομής της ωλένης και η κεφαλή της κερκίδας πρέπει να σχηματίζουν τόξο με ομαλό περίγραμμα (εικόνα 2).
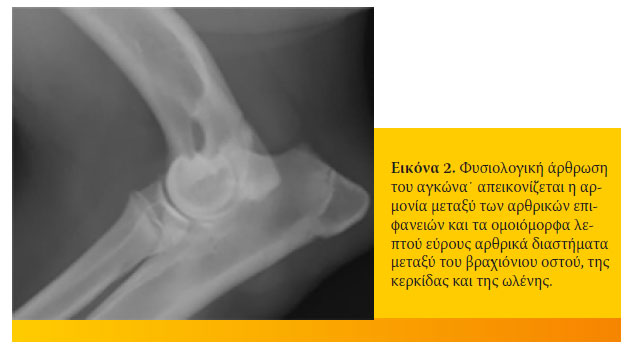
Στη θέση αυτή, σε σκύλο με δυσπλασία του αγκώνα ηλικίας μικρότερης του ενός έτους, μπορεί να απεικονιστούν ένα ή και περισσότερα από τα ακόλουθα παθολογικά ευρήματα:
- Διεύρυνση του αρθρικού διαστήματος της βραχιονιωλενικής διάρθρωσης στο κεντρικό τμήμα της τροχιλιακής εντομής.
- Διεύρυνση του αρθρικού διαστήματος της βραχιονιοκερκιδικής διάρθρωσης.
- Διακοπή του ομαλού περιγράμματος του τόξου που σχηματίζεται από την τροχιλιακή εντομή της ωλένης και την αρθρική επιφάνεια της κερκίδας. Το παθολογικό αυτό εύρημα ονομάζεται «σκαλοπάτι».34
- Κάταγμα της έσω κορωνοειδούς απόφυσης, το οποίο μπορεί να είναι απλό ή με τη μορφή πολλαπλών παρασχίδων της έσω κορωνοειδούς απόφυσης. Η φυσιολογική έσω κορωνοειδής απόφυση απεικονίζεται ως μια τριγωνική περιοχή υποχόνδριου οστού, με οξύαιχμη περιφέρεια, που συμπροβάλλεται με την κεφαλή της κερκίδας. Το κάταγμα της έσω κορωνοειδούς απόφυσης απεικονίζεται σε ποσοστό μόλις 9,8% των περιστατικών.
- Ήπια αύξηση της οστικής πυκνότητας (οστεοσκλήρυνση) και απώλεια των οστικών δοκίδων στο περιφερικό άκρο της τροχιλιακής εντομής. Το ακτινογραφικό αυτό εύρημα, αποτελεί πρώιμη ένδειξη άσκησης μη φυσιολογικών φορτίσεων στην άρθρωση του αγκώνα (εικόνα 3).
- Παρουσία οστεοφύτων στη ραχιαία επιφάνεια του ράμφους του ωλεκράνου. Σε σκύλους ηλικίας μεγαλύτερης του ενός έτους, οι αλλοιώσεις της δευτερογενούς οστεοαρθρίτιδας συχνά επεκτείνονται και στο πρόσθιο αρθρικό χείλος της κεφαλής της κερκίδας.
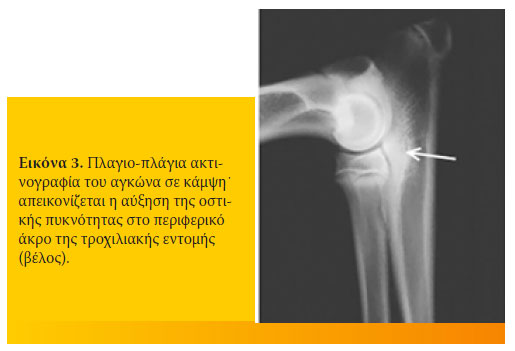
Β. Πλαγιο-πλάγια ακτινογραφία με την άρθρωση του αγκώνα σε κάμψη.
Στη θέση αυτή, η γωνία μεταξύ του βραχιόνιου οστού και του αντιβραχίου πρέπει να είναι περίπου 45ο. Το άκρο τοποθετείται έτσι, ώστε οι κόνδυλοι του βραχιόνιου οστού να συμπροβάλλονται στο ακτινογραφικό φιλμ. Η θέση αυτή είναι ειδική για τη διάγνωση της ΑΣΡΩ, επειδή έχει το πλεονέκτημα έναντι της πλαγιο-πλάγιας προβολής με την άρθρωση του αγκώνα σε έκταση, να αποφεύγεται η συμπροβολή του έσω επικόνδυλου του βραχιόνιου οστού με το ράμφος του ωλεκράνου. Έτσι, είναι ευκρινής η απεικόνιση του ράμφους, καθώς και των οστεφύτων στη ραχιαία επιφάνεια του ωλεκράνου.
Στους σκύλους μεγαλόσωμων φυλών το ράμφος του ωλεκράνου έχει δικό του δευτερογενή πυρήνα οστέωσης. Ο συζευκτικός χόνδρος του πυρήνα αυτού οστέωσης του ράμφους του ωλεκράνου απεικονίζεται ακτινογραφικά μέχρι την ηλικία των 3½ - 5½ μηνών. Η ακτινογραφική απεικόνιση του συζευκτικού χόνδρου μετά την ηλικία αυτή θεωρείται παθογνωμονικό εύρημα ΑΣΡΩ. Ο παραμένων συζευκτικός χόνδρος απεικονίζεται ως ένα ακτινοδιαυγές διάστημα με ασαφή όρια, μεταξύ του ράμφους του ωλεκράνου και του ωλεκράνου (εικόνα 4).
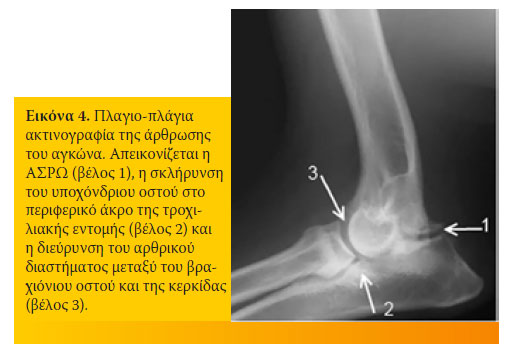
Γ. Προσθιο-οπίσθια ακτινογραφία της άρθρωσης του αγκώνα.
Στη λήψη αυτή, ο σκύλος τοποθετείται σε στερνική κατάκλιση και το προς ακτινογράφηση άκρο συγκρατείται με, το βραχιόνιο οστό κάθετο προς στον άξονα της σπονδυλικής στήλης, η άρθρωση του αγκώνα σε επαφή με την στην ακτινογραφική κασέτα και το αντιβράχιο σε έκταση προς τα εμπρός.
Στη θέση αυτή απεικονίζεται η χαρακτηριστική αλλοίωση της ΔΟ ήδη από την ηλικία των 5-6 μηνών, ως μία ακτινοδιαφανής περιοχή ή ως επιπέδωση ή ακόμη και ως έλλειμμα στο υποχόνδριο οστό της αρθρικής επιφάνειας της τροχιλίας του βραχιόνιου οστού.33
Δ. Λοξή προσθιοεξωτερική – οπισθιοεσωτερική ακτινογραφία (-150) του αγκώνα.
Σε αυτή τη λήψη ο σκύλος τοποθετείται σε στερνική κατάκλιση και το προς ακτινογράφηση άκρο του φέρεται σε θέση όπως στην προσθιο-οπίσθια ακτινογράφηση με το αντιβράχιο όμως να στρέφεται προς τα έσω (πρηνισμός) κατά 150. Η ακτινογραφική δέσμη επικεντρώνεται στο κέντρο της άρθρωσης του αγκώνα. Στη θέση αυτή απεικονίζεται ευκρινέστερα η αρθρική επιφάνεια της τροχιλίας του βραχιόνιου οστού και η έσω κορωνοειδής απόφυση.
> Σύγχρονες θεραπευτικές επιλογές
Η αντιμετώπιση της δυσπλασίας του αγκώνα είναι χειρουργική και πρέπει να γίνεται πριν την εγκατάσταση αλλοιώσεων οστεοαρθρίτιδας στην άρθρωση. Εάν η χειρουργική αντιμετώπιση καθυστερήσει δεν μπορεί να ελεγχθεί συνήθως η εξέλιξη της οστεοαρθρίτιδας. Δυστυχώς, η πολυπλοκότητα της παθογένειας, των κλινικών συμπτωμάτων και των απεικονιστικών ευρημάτων, καθιστά τη διάγνωση των πρώιμων σταδίων της νόσου δύσκολη.
Οι χειρουργικές τεχνικές αντιμετώπισης της δυσπλασίας του αγκώνα που περιγράφονται στην εργασία αυτή ταξινομούνται σε χειρουργικές τεχνικές για την αντιμετώπιση της ΝΕΤΑ σε σκύλους με ελαφριάς μορφής οστεοαρθρίτιδα, σε χειρουργικές τεχνικές για την αντιμετώπιση της ΝΕΤΑ σε σκύλους με μέτριας ή βαριάς μορφής οστεοαρθρίτιδα και σε χειρουργικές τεχνικές για την αντιμετώπιση της αδυναμίας συνοστέωσης του ράμφους του ωλεκράνου.44
1. Χειρουργικές τεχνικές αντιμετώπισης ΝΕΤΑ σε σκύλους με ελαφριά οστεοαρθρίτιδα.
α. ΝΕΚΑ.
Μολονότι για την επιλογή της κατάλληλης μεθόδου αντιμετώπισης της ΝΕΚΑ έχουν γίνει αρκετές έρευνες, μέχρι σήμερα δεν υπάρχει ομόφωνη άποψη για τη μέθοδο εκλογής. Τα αποτελέσματα των ερευνών ποικίλουν, όμως στις περισσότερες από αυτές περιγράφεται φυσιολογική λειτουργία του άκρου για βραχύ χρονικό διάστημα μετά τη χειρουργική αντιμετώπιση και επιδείνωση της οστεοαρθρίτιδας σε μεσοχρόνια ή μακροχρόνια βάση.37,38 Ορισμένοι μάλιστα συγγραφείς αναφέρουν, ότι η χειρουργική αντιμετώπιση δεν μεταβάλει τη μακροχρόνια πρόγνωση και προτιμούν να αντιμετωπίζουν τη ΝΕΚΑ συντηρητικά.39
Οι χειρουργικές τεχνικές που αναφέρονται στην αντιμετώπιση της ΝΕΚΑ ταξινομούνται σε δύο κατηγορίες. Στην πρώτη κατηγορία κατατάσσονται οι εστιακές τεχνικές, στις οποίες η προσπέλαση μπορεί να γίνει με αρθροτομή ή με αρθροσκόπιο, ενώ στη δεύτερη κατηγορία κατατάσσεται η οστεκτομή της ωλένης, που μπορεί να πραγματοποιηθεί σε συνδυασμό με τις εστιακές τεχνικές.
Από τις εστιακές τεχνικές, έχουν μελετηθεί περισσότερο η απομάκρυνση του αποσπασμένου ή των αποσπασμένων τμημάτων της έσω κορωνοειδούς απόφυσης της ωλένης, καθώς και η μερική οστεκτομή της έσω κορωνοειδούς απόφυσης της ωλένης.
Η απομάκρυνση του αποσπασμένου ή των αποσπασμένων τμημάτων της έσω κορωνοειδούς απόφυσης της ωλένης οδηγεί πάντοτε σε οστεοαρθρίτιδα και διατήρηση της χωλότητας, διότι παραμένουν οι εκφυλιστικές αλλοιώσεις στο υποχόνδριο οστό. Για το λόγο αυτό προτάθηκε η ταυτόχρονη μερική οστεκτομή μεγάλου τμήματος της έσω κορωνοειδούς απόφυσης της ωλένης, στο οποίο περιλαμβάνεται το μεγαλύτερο τμήμα του πάσχοντος υποχόνδριου οστού28,40,41 (εικόνα 5).
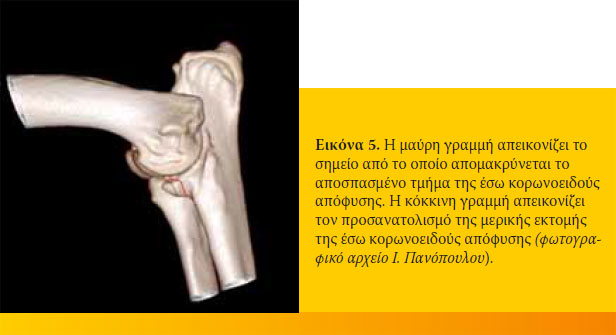
Η μερική οστεκτομή της έσω κορωνοειδούς απόφυσης της ωλένης, η οποία μπορεί να γίνει με οστεοτόμο ή με αεροπρίονο, έχει φορά από το οπίσθιο-εσωτερικό όριο της έσω κορωνοειδούς απόφυσης προς το πρόσθιο-εξωτερικό όριο της κερκιδικής εντομής της ωλένης. Από το οστεοτομημένο οστικό τεμάχιο απομακρύνονται οι προσφύσεις του δακτυλιοειδή συνδέσμου και αυτό απομακρύνεται.42,43 Ακολουθεί πλύση της άρθρωσης με φυσιολογικό ορό, έγχυση στην αρθρική κοιλότητα διαλύματος μπουπιβακαΐνης 0,5% σε δόση 1 mg/kg ΣΒ και συρραφή του εγχειρητικού τραύματος.
Δεν έχουν γίνει επαρκείς συγκριτικές μελέτες των αποτελέσματων της μερικής οστεκτομής της έσω κορωνοειδούς απόφυσης της ωλένης και της απλής απομάκρυνσης των αποσπασμένων τμημάτων της έσω κορωνοειδούς απόφυσης. Ως εκ τούτου, απαιτείται μεγαλύτερη έρευνα για τον προσδιορισμό των ενδείξεων και της μετεγχειρητικής εξέλιξης από την εφαρμογή των παραπάνω τεχνικών στην καθημερινή πράξη.43
Στην περίπτωση που η ΝΕΚΑ συνυπάρχει με το σύνδρομο της βραχείας κερκίδας, και προκειμένου να αντιμετωπιστούν οι μεγάλες φορτίσεις στο εσωτερικό τμήμα της άρθρωσης, η εστιακή αντιμετώπιση συνδυάζεται με κεντρική οστεκτομή της ωλένης.44
Συχνά η ΝΕΚΑ συνοδεύεται με αλλοίωση του αρθρικού χόνδρου της τροχιλίας του βραχιόνιου οστού, η θεραπεία του οποίου συνίσταται στην απομάκρυνση του ελεύθερου τμήματός του και στην νεαροποίηση της περιοχής.
β. Σύνδρομο βραχείας κερκίδας
Η αντιμετώπιση του συνδρόμου της βραχείας κερκίδας έχει σκοπό την αποκατάσταση της αρμονίας στις αρθρικές επιφάνειες της κερκιδωλενικής διάρθρωσης, εξαλείφοντας την διαφορά ύψους μεταξύ των αρθρικών επιφανειών της κερκίδας και της ωλένης. Ο σκοπός αυτός επιτυγχάνεται χειρουργικά με κεντρική οστεκτομή της ωλένης.25,45
Μετά την οστεκτομή της ωλένης, από το βάρος του σώματος ωθείται η αρθρική επιφάνεια της ωλένης περιφερικά, με αποτέλεσμα η αρθρική επιφάνεια της κερκίδας και της ωλένης να ευθυγραμμίζονται στο ίδιο επίπεδο. Η τεχνική εφαρμόζεται όταν στην πλαγιο-πλάγια ακτινογραφία της άρθρωσης του αγκώνα η διαφορά ύψους («σκαλοπάτι») μεταξύ των αρθρκών επιφανειών κερκίδας και ωλένης είναι μεγαλύτερη από 2 mm.
Η οστεκτομή της ωλένης γίνεται με την εκτέλεση δύο παράλληλων οστεοτομών στην ωλένη, οι οποίες έχουν απόσταση η μία από την άλλη ίση με τη διαφορά ύψους των αρθρικών επιφανειών κερκίδας – ωλένης όπως αυτή απεικονίζεται στην πλάγιο-πλάγια ακτινογραφία. Οι οστεοτομές έχουν λοξή φορά σε σχέση με τον επιμήκη άξονα της ωλένης και η κατεύθυνσή τους είναι από οπίσθιο-κεντρικά προς πρόσθιο-περιφερικά με γωνία 400 σε σχέση με τον επιμήκη άξονα και από κέντρο-εσωτερικά προς περιφέρικο-εξωτερικά με γωνία 500 σε σχέση με τον επιμήκη άξονα (εικόνα 6).20
Η ευθυγράμμιση της οστεοτομημένης ωλένης μπορεί να διασφαλιστεί με ενδομυελικό ήλο.46

γ. Στροφική αστάθεια της κερκιδωλενικής διάρθρωσης.
Για την εξουδετέρωση της διατμητικής δύναμης μεταξύ της κερκίδας και της ωλένης, η οποία δημιουργείται κατά την κάμψη της άρθρωσης του αγκώνα λόγω της υφιστάμενης δυσαρμονίας μεταξύ της οπίσθιας αρθρικής επιφάνειας της κερκίδας με την κερκιδική εντομή της ωλένης, σε συνδυασμό με την έκκεντρη θέση των καταφύσεων των τενόντων του δικέφαλου βραχιόνιου και του πρόσθιου βραχιόνιου μυ σε σχέση με τον ανατομικό άξονα του αντιβραχίου, δημοσιεύτηκε πρόσφατα χειρουργική τεχνική απελευθέρωσης των καταφυτικών τενόντων του δικέφαλου βραχιόνιου και του πρόσθιου βραχιόνιου μυ από την ωλένη (biceps-brachial ulnar release procedure, BURP).27
Ο καταφυτικός τένοντας του δικέφαλου βραχιόνιου μυ είναι δισχιδής. Ο ένας κλάδος καταφύεται στο κερκιδικό όγκωμα (εσωτερικό τμήμα της πρόσθιας μοίρας του άνω άκρου της κερκίδας), ενώ ο άλλος κλάδος, μαζί με τον καταφυτικό τένοντα του πρόσθιου βραχιόνιου μυ καταφύονται, υπό μορφή ευρείας «βεντάλιας», στο ωλένιο όγκωμα (ενδοαρθρική εσωτερική επιφάνεια της κορωνοειδούς απόφυσης). Κατά την τεχνική της απελευθέρωσης των καταφυτικών τενόντων του δικέφαλου βραχιόνιου και πρόσθιου βραχιόνιου μυ από την ωλένη, εκτελείται τενοντοτομή των καταφυτικών τενόντων στο σημείο της κατάφυσής τους στην εσωτερική επιφάνεια της έσω κορωνοειδούς απόφυσης. Η προσπέλαση στο σημείο κατάφυσης των τενόντων γίνεται με ελάχιστα επεμβατική αρθροτομή ή με αρθροσκόπιο.
Η BURP ενδείκνυται σε σκύλους νεαρής ηλικίας, με χωλότητα και πόνο κατά την ψηλάφηση της άρθρωσης, στους οποίους τόσο απεικονιστικά ή και αρθροσκοπικά διαπιστώνεται ότι ο βαθμός της κάκωσης του αρθρικού χόνδρου και του υποχόνδριου οστού είναι μικρός (μικρός αριθμός ρωγμών και ελαφρού βαθμού σκλήρυνση στο υποχόνδριο οστό της περιοχής της κερκιδικής εντομής της ωλένης).28
Η κάμψη της άρθρωσης του αγκώνα δεν επηρεάζεται μετά τη χειρουργική επέμβαση, επειδή η δεύτερη κατάφυση του τένοντα του δικέφαλου βραχιόνιου μυ στην κερκίδα παραμένει ανέπαφη.
δ. Διαχωριστική οστεοχονδρίτιδα.
Η κλασσική χειρουργική αντιμετώπιση της ΔΟ της τροχιλίας του βραχιόνιου οστού συνίσταται στην απομάκρυνση τόσου του ελεύθερου τμήματος του αρθρικού χόνδρου, όσο και του τμήματος του αρθρικού χόνδρου από την περιφέρεια της αλλοίωσης, με σκοπό την απομάκρυνση της εστίας της φλεγμονής από την άρθρωση. Στη συνέχεια, τα χείλη της περιφέρειας της αλλοίωσης στρογγυλοποιούνται, για να μην αναχαιτιστεί η πλήρωση του ελλείμματος με ινοχόνδρινο ιστό.47 Πριν από τη συρραφή του αρθρικού θυλάκου, η άρθρωση εκπλύνεται με άφθονο φυσιολογικό ορό για την απομάκρυνση των ιζημάτων τριβής του ελεύθερου τμήματος του αρθρικού χόνδρου.
Για την διέγερση και την επιτάχυνση της επούλωσης του αρθρικού χόνδρου, μετά την αφαίρεση του ελεύθερου τμήματός του, έχουν περιγραφεί τεχνικές ανάπλασης και τεχνικές αποκατάστασης του χόνδρου.
Οι τεχνικές ανάπλασης του χόνδρου έχουν σκοπό τη δημιουργία καναλιών διείσδυσης του αίματος, από το υποκείμενο οστό στη θέση του ελλείμματος. Η είσοδος αίματος στο έλλειμμα παρέχει αιμοποιητικά και μεσεγχυματικά προγονικά κύτταρα, καθώς και παράγοντες ανάπτυξης, για την επιτάχυνση της επούλωσης και τη βελτίωση της ποιότητας του δημιουργούμενου ινοχόνδρινου ιστού, ώστε να προσομοιάζει περισσότερο με υαλώδη χόνδρο. Στις τεχνικές ανάπλασης περιλαμβάνονται η απόξεση και η οστεοπαρακέντηση.
Απόξεση είναι η αφαίρεση με κοχλιάριο απόξεσης του χαλαρού και νεκρωμένου χόνδρου, καθώς και του πάσχοντος υποχόνδριου οστού, μέχρι την αποκάλυψη υγιούς οστού που αιμορραγεί. Το κύριο μειονέκτημα της απόξεσης είναι η εκτεταμένη κάκωση του υποχόνδριου οστού, καθώς και η δημιουργία αλλοίωσης μεγάλης έκτασης και βάθους, με συνέπεια την καθυστέρηση της επούλωσης και τη δημιουργία ινοχόνδρινου ιστού κακής ποιότητας.
Η οστεοπαρακέντηση συνίσταται στην δημιουργία πολυάριθμων οπών στο υποχόνδριο οστό με λεπτό ήλο Kirschner, μέχρι την εμφάνιση αίματος. Σε σύγκριση με την τεχνική της απόξεσης η βλάβη του υποχόνδριου οστού είναι μικρότερη.
Οι τεχνικές αποκατάστασης του αρθρικού χόνδρου έχουν σκοπό την αποκατάσταση του ελλείμματος με υαλώδη χόνδρο. Αυτό επιτυγχάνεται με την τοποθέτηση στο έλλειμμα οστεοχόνδρινου αυτομοσχεύματος. Ειδικότερα, μετά την απομάκρυνση του οστεοχόνδρινου ελεύθερου τμήματος, δημιουργούνται σημεία υποδοχής του οστεοχόνδρινου μοσχεύματος, με το οποίο θα καλυφτεί η αλλοίωση (OATS, Arthex, Naples, FL). Το οστεοχόνδρινο αυτομόσχευμα συλλέγεται με ειδική τεχνική από την αρθρική επιφάνεια της άρθρωσης του γόνατος.1
2. Χειρουργικές τεχνικές αντιμετώπισης της ΝΕΤΑ, σε σκύλους με μέτρια ή βαριά οστεοαρθρίτιδα.
Οι σύγχρονες τεχνικές, οι οποίες εφαρμόζονται σε περίπτωση αλλοιώσεων οστεοαρθρίτιδας μόνο στο εσωτερικό τμήμα της άρθρωσης είναι η συρταρωτή οστεοτομία του βραχιόνιου οστού (sliding humeral osteotomy, SHO) και η κεντρική οστεοτομία της ωλένης και ακινητοποίηση στη συνέχεια των καταγματικών τμημάτων σε θέση πρόκλησης απαγωγής του άκρου (proximal abducting ulnar osteotomy, PAUL). Σκοπός των τεχνικών αυτών είναι η μείωση των ασκούμενων φορτίσεων στο πάσχον εσωτερικό τμήμα της άρθρωσης και η μεταφορά των φορτίσεων στο υγιές εξωτερικό τμήμα.
Κατά την τεχνική SHO, εκτελείται εγκάρσια οστεοτομή στο μέσο της διάφυσης του βραχιόνιου οστού και τα δύο καταγματικά τμήματα ακινητοποιούνται σε νέα θέση με αυτασφαλιζόμενη μεταλλική πλάκα, στο μέσον της οποίας υπάρχει «σκαλοπάτι». Με τη βοήθεια της παραπάνω ειδικής μεταλλικής πλάκας το περιφερικό τμήμα της διάφυσης του βραχιόνιου οστού μετατοπίζεται προς τα έσω, σε σχέση με το μηχανικό άξονα βραχιόνιου οστού – αντιβραχίου. Η μετατόπιση του μηχανικού αυτού άξονα έχει ως αποτέλεσμα, την αποφόρτιση του πάσχοντος αρθρικού χόνδρου της βραχιονωλενικής διάρθρωσης και τη φόρτιση του φυσιολογικού αρθρικού χόνδρου της βραχιονιοκερκιδικής διάρθρωσης (εικόνες 7α & 7β).48,49

Σε μία μελέτη 59 περιστατικών δυσπλασίας αγκώνα, τα οποία χειρουργήθηκαν με την τεχνική της SHO διαπιστώθηκε καλή έως άριστη μεσοχρόνια μετεγχειρητική εξέλιξη.49 Αναλυτικότερα, 26 εβδομάδες μετά τη χειρουργική επέμβαση, σε ποσοστό 65,6% των περιπτώσεων δεν παρατηρήθηκε χωλότητα, ενώ σε ποσοστό 31,3% η χωλότητα ήταν ήπιου βαθμού. Ωστόσο, έχουν αναφερθεί βαριές επιπλοκές, με τη συγκράτηση της μεταλλικής πλάκας στο βραχιόνιο οστό και εκτιμάται ότι απαιτούνται και άλλες μελέτες με μεγαλύτερο αριθμό περιστατικών για τον έλεγχο της μετεγχειρητικής πορείας σε μακρύτερο διάστημα, πριν από την καθιέρωση της τεχνικής αυτής στην καθημερινή πράξη.
Κατά τη νεότερη τεχνική PAUL εκτελείται οστεκτομή στο κεντρικό τμήμα της ωλένης και τα δύο καταγματικά τμήματα ακινητοποιούνται σε νέα θέση με ειδική αυτασφαλιζόμενη μεταλλική πλάκα, στο μέσον της οποίας υπάρχει «σκαλοπάτι» ύψους 2 ή 3 mm (KYON, Zurich, Switzerland) (εικόνα 8).50 Στη νέα αυτή θέση η ωλένη προκαλεί απαγωγή του αντιβραχίου, με συνέπεια τη μεταφορά των φορτίσεων του βάρους του σώματος στο εξωτερικό τμήμα της άρθρωσης του αγκώνα και την ανακούφιση του εσωτερικού τμήματος (εικόνα 9). Μολονότι η τεχνική αυτή υπόσχεται καλά αποτελέσματα δεν έχει γίνει μέχρι σήμερα μεγάλη αναλυτική μελέτη του ποσοστού της επιτυχίας και των επιπλοκών από την εφαρμογή της.

Όταν και στα δύο τμήματα της άρθρωσης του αγκώνα υπάρχουν βαριές αλλοιώσεις οστεοαρθρίτιδας, οι χειρουργικές θεραπευτικές επιλογές είναι η αρθρόδεση ή η ολική αντικατάσταση της άρθρωσης.
Με την αρθρόδεση της άρθρωσης του αγκώνα επιτυγχάνεται ανακούφιση από τον πόνο της χρόνιας οστεοαρθρίτιδας, προκαλείται όμως σημαντική απώλεια της λειτουργικότητας του άκρου.49
Η ολική αρθροπλαστική της άρθρωσης του αγκώνα μολονότι έχει αρχίσει να μελετάται για περισσότερα από 10 χρόνια, δεν εφαρμόζεται συχνά στην πράξη, λόγω της μεγάλης τεχνικής δυσκολίας, του υψηλού ποσοστού επιπλοκών και της απρόβλεπτης μετεγχειρητικής πορείας.51 Η ολική αρθροπλαστική του αγκώνα θα πρέπει να επιχειρείται μόνο σε αρθρώσεις με πολύ βαριά οστεοαρθρίτιδα, και ύστερα από ενημέρωση των ιδιοκτητών για το ενδεχόμενο μεγάλο ποσοστό επιπλοκών.
3. Χειρουργικές τεχνικές αντιμετώπισης της ΑΣΡΩ.
Η ΑΣΡΩ είναι δυνατόν να αντιμετωπιστεί χειρουργικά με τρεις διαφορετικές τεχνικές, δηλαδή με κεντρική οστεοτομή της ωλένης, με αφαίρεση του ράμφους του ωλεκράνου και με ακινητοποίηση του ράμφους του ωλεκράνου στην ωλένη με κοχλία συμπίεσης.52
Με την κεντρική οστεοτομή της ωλένης προκαλείται κεντρική μετακίνηση του κεντρικού τμήματος της ωλένης από την έλξη του τρικέφαλου βραχιόνιου μυ, με συνέπεια την αποκατάσταση της ευθυγράμμισης των αρθρικών επιφανειών της κερκίδας και της ωλένης και την ανακούφιση του ράμφους του ωλεκράνου από τα φορτία που ασκούνται σε αυτό από τον κόνδυλο του βραχιόνιου οστού.23,53 Η κατεύθυνση της οστεοτομής είναι όμοια με την κατεύθυνση της κεντρικής οστεκτομής της ωλένης. Τα δύο τμήματα της ωλένης αφήνονται ελεύθερα ή και ακινητοποιούνται με ενδομυελικό ήλο.
Η τεχνική της ακινητοποίησης του ράμφους του ωλεκράνου στην ωλένη με κοχλία συμπίεσης εφαρμόζεται σε σκύλους ηλικίας μικρότερης των 6 μηνών, στους οποίους η τροχιλιακή εντομή είναι φυσιολογική.
Βιβλιογραφικά, τα καλύτερα μετεγχειρητικά αποτελέσματα έχουν αναφερθεί με την τεχνική της ακινητοποίησης του ράμφους του ωλεκράνου στην ωλένη, σε συνδυασμό με την κεντρική οστεοτομή της ωλένης.54
> Συμπεράσματα
Σήμερα υποστηρίζεται ότι κύρια αιτία της δυσπλασίας του αγκώνα είναι η ΔΑ, μολονότι σε μερικούς σκύλους εμπλέκεται και η ΔΟ. Η συχνότερη μορφή δυσαρμονίας είναι η διαφορά μήκους της κερκίδας και της ωλένης, κατά την οποία, η κεφαλή της κερκίδας βρίσκεται σε χαμηλότερο ή υψηλότερο επίπεδο από την έσω κορωνοειδή απόφυση της ωλένης, μεταφέροντας έτσι μεγάλες φορτίσεις στο ράμφος του ωλεκράνου ή στην έσω κορωνοειδή απόφυση αντίστοιχα. Θεωρείται, ότι ο ακριβής παθογενετικός μηχανισμός είναι περίπλοκος και δεν έχει ακόμα πλήρως διευκρινιστεί.
Για την οριστική διάγνωση απαιτούνται απεικονιστικές εξετάσεις ή και αρθροσκόπηση. Η αξονική τομογραφία έχει μεγαλύτερη ειδικότητα και ευαισθησία για τη διάγνωση της δυσπλασίας του αγκώνα από την απλή ακτινογράφηση.
Η χειρουργική θεραπεία της δυσπλασίας του αγκώνα πρέπει να γίνεται πριν από την εμφάνιση βαριών αλλοιώσεων οστεοαρθρίτιδας. Στις χειρουργικές τεχνικές περιλαμβάνονται η μερική εκτομή της έσω κορωνοειδούς απόφυσης και η αποκατάσταση της διαφοράς μήκους μεταξύ των αρθρικών επιφανειών της κερκίδας και της ωλένης με την εκτέλεση οστεκτομής ή οστεοτομίας. Εάν οι αλλοιώσεις στην άρθρωση του αγκώνα είναι βαριές και αφορούν μόνο στο εσωτερικό τμήμα, εφαρμόζονται οι τεχνικές SHO ή PAUL. Στην περίπτωση που υπάρχουν αλλοιώσεις σε ολόκληρη την άρθρωση του αγκώνα, συνιστάται η ολική αντικατάσταση της άρθρωσης ή η αρθρόδεση. Με την αρθρόδεση αντιμετωπίζεται ο πόνος, αλλά παραμένουν βαριά λειτουργικά προβλήματα.
Η πλήρης κατανόηση της παθογένειας της δυσπλασίας του αγκώνα θα καταστεί δυνατή μόνον εάν γίνει έρευνα ανάλυσης και επεξεργασίας των δεδομένων της βάδισης με υπολογιστικές τεχνικές. Τότε πιθανόν να αναθεωρηθούν όλες οι χειρουργικές επιλογές και να προκύψουν νέες, για τη θεραπεία μιας συχνής νόσου που προκαλεί χρόνιο πόνο και καταβάλει σε μεγάλο βαθμό τους πάσχοντες σκύλους.
> Ευχαριστίες
Οι συγγραφείς ευχαριστούν το συνάδελφο Ιωάννη Πανόπουλο για την παραχώρηση φωτογραφιών από το προσωπικό του αρχείο.
> Βιβλιογραφία
1. Griffon DJ. Surgical diseases of the elbow. In: Small Animal Veterinary Surgery. Tobias KM, Johnson SA (eds). Elsevier Saunders, St Louis, MO, USA, 2012, pp.724-759.
2. Hazewinkel HAW, Meij BP, Nap RC, Ubbink GJ. Radiographic views for elbow dysplasia screening in Bernese Mountain dogs. Proceedings International Elbow Working Group 1995, 5: 32-37.
3. Morgan JP, Wind A, Davidson AP. Bone dysplasias in the labrador retriever: a radiographic study. J Am Anim Hosp Assoc 1999, 35: 332–340.
4. Morgan JP, Wind A, Davidson AP. Elbow Dysplasia. In: Hereditary Bone and Joint Diseases in the Dog. Morgan JP and Davidson AP, (eds). 1st ed. Hannover Schultersche: Germany, 2000, pp. 41-68.
5. Meyer-Lindberg A, Fehr M, Nolte I. Co-existance of UAP and FCP of the ulna in the dog. J Small Anim Pract 2006, 47: 61–65.
6. Kirberger RM, Fourie SL. Elbow dysplasia in the dog: pathophysiology, diagnosis and control. J S Afr Vet Assoc 1998, 69: 43–54.
7. Vermote KA, Bergenhuyzen AL, Gielen I, van Bree H, Duchateau L, Van Ryssen B. Elbow lameness in dogs of six years and older. arthroscopic and imaging findings of medial coronoid disease in 51 dogs. Vet Comp Orthop Traumatol 2010, 23: 43–50.
8. Snaps FR, Balligand MH, Saunders JH, Park RD, Dondelinger RF. Comparison of radiography, magnetic resonance imaging and surgical findings in dogs with elbow dysplasia. Am J Vet Res 1997, 58: 1367-1370.
9. Michelsen J. Canine Elbow dysplasia: aetiopathogenesis and current treatment recommendations. Vet J 2013, 196:12- 19.
10. Clements DN. Gene expression in normal and diseased elbows. In: Proceedings of the Autumn Meeting of the British Veterinary Orthopaedic Association: Chester, UK, 2006, pp. 6–7.
11. Grandalen J, Lingaas F. Arthrosis in the elbow joint of young rapidly growing dogs: A genetic investigation. J Small Anim Pract 1991, 32: 460–464.
12. Lewis TW, Ilska JJ, Blott SC, Woolliams JA. Genetic evaluation of elbow scores and the relationship with hip scores in UK Labrador retrievers. Vet J 2011, 189: 227–233.
13. Nap RC. Pathophysiology and clinical aspects of canine elbow dysplasia. In: Proceedings of the 7th International Elbow Working Group Meeting, Constance, Germany, 1995, pp. 6–8.
14. Olsson SE. The early diagnosis of fragmented coronoid process and osteochondritis dissecans of the canine elbow joint. J Am Anim Hosp Assoc 1983, 19: 616–626.
15. Gemmill TJ, Mellor DJ, Clements DN, Clarke SP, Farrell M, Bennett D, Carmichael S. Evaluation of elbow incongruency using reconstructed CT in dogs suffering fragmented coronoid process. J Small Anim Pract 2005, 46: 327–333.
16. Kramer A, Holsworthy IG, Wisner ER, Kass PH, Schultz KS. Computed tomographic evaluation of canine radioulnar incongruence in vivo. Vet Surg 2006, 35: 24–29.
17. Hulse D. Co-contraction of the biceps/brachialis muscle complex produces a rotational moment which may induce fragmentation/microfracture of the medial coronoid. In: Congress proceedings of the American College of Veterinary Surgeons Symposium: San Diego, USA, 2008, pp. 466.
18. Bennett D, Duff SR, Kene RO, Lee R. Osteochondritis dissecans and fragmentation of the coronoid process in the elbow joint of the dog. Vet Rec 1981, 109: 329–336.
19. Guthrie S, Plummer JM, Vaughan LC. Post natal development of the canine elbow joint: a light and electron microscopic study. Res Vet Sci 1992, 52: 67-71. 20. Burton, NJ, Owen MR. Canine elbow dysplasia 2. Treatment and prognosis. In Practice 2008, 30: 552–557.
21. Bottcher P. Radio-ulnar incongruence in dogs with elbow dysplasia. In: Congress proceedings of the American College of Veterinary Surgeons Symposium, Chicago, USA, 2011b, pp. 110–112.
22. Preston, CA, Schulz KS, Kass PH. In vitro determination for contact areas in the normal elbow joint of dogs. Am J Vet Res 2000, 61: 1315–1321.
23. Sjstrom L, Kasstom H, Kllber M. Ununited anconeal process in the dog. Pathogenesis and treatment by osteotomy of the ulna. Vet Comp Orthop Traumatol 1995, 8: 170–176.
24. Lozier SM. How I treat elbows in the older canine patient and new prospective in elbow dysplasia. In: Congress proceedings of the 13th European Society of Veterinary Orthopaedics and Traumatology: Munich, Germany, 2006, pp. 93–96.
25. Wind AP, Packard ME. Elbow incongruity and developmental elbow diseases in the dog. Part II. J Am Anim Hosp Assoc 1986, 22: 725–730.
26. Proks P, Necas A, Stehlik L, Srnec R, Griffon DJ. Quantification of humeroulnar incongruity in Labrador retrievers with and without medial coronoid disease. Vet Surg 2011, 40: 981–986.
27. Fitzpatrick N. Biceps ulnar release procedure for treatment of medial coronoid disease in 49 elbows. In: Congress proceedings of the 36th Annual Conference, Veterinary Orthopaedic Society, Steamboat Springs: Colorado, USA, 2009, p. 44.
28. Fitzpatrick, N, Yeadon R. Working algorithm for treatment decision making for developmental disease of the medial compartment of the elbow in dogs. Vet Surg 2009, 38: 285–300.
29. Trostel C, McLaughlin R, Pool R. Canine lameness caused by developmental orthopedic diseases: FCP and UAP. Compend Cont Educ Pract 2003, 25: 112.
30. Demko J, McLaughlin R. Developmental orthopedic disease. Vet Clin North Am 2005, 35: 1111-1135.
31. Punke JP, Hulse DA, Kerwin SC, Peycke LE, Budsberg SC. Arthroscopic documentation of elbow cartilage pathology in dogs with clinical lameness without changes on standard radiographic projections. Vet Surg 2009, 38: 209
32. Boulay JP. Fragmented medial coronoid process of the ulna in the dog. Vet Clin North Am 1998, 28: 449-458.
33. Henry WB. Radiographic diagnosis and surgical management of fragmented medial coronoid process in dogs. J Am Vet Med Assoc 1984, 184: 799-805.
34. Wosar M, Lewis D, Neuwirth L, Parker RB, Spencer CP, Kubilis PS, Stubbs WP, Murphy ST, Shiroma JT, Stallings JT, Bertrand SG. Radiographic evaluation of elbow joints before and after surgery in dogs with possible fragmented medial coronoid process. J Am Vet Med Assoc 1999, 214: 52-58.
35. Rovesti G, Biasibetti M, Schumacher A, Fabiani M. The use of CT in the diagnostic protocol of the elbow in the dog: 24 joints. Vet Comp Orthop Traumatol 2002, 15: 35-39.
36. Carpenter LG, Schwarz PD, Lowry JE, Steyn PF. Comparison of radiologic imaging techniques for diagnosis of FCP of the cubital joint in dogs. J Am Vet Med Assoc 1993, 203: 78-83.
37. Ness M. Treatment of FCP in young dogs by proximal ulnar osteotomy. J Small Anim Pract 1998, 39:15-21.
38. Read RA, Armstrong SJ, O’Keef D, Eger CE. Fragmentation of the medial coronoid process of the ulna in dogs: a study of 109 cases. J Small Anim Pract 1990, 31: 330-334.
39. Book GR, Miller CW, Tavers CL. A comparison of surgical and medical treatment of fragmented coronoid process and osteochondritis dissecans of the canine elbow. Vet Comp Orthop Traumatol 1995, 8: 117-120.
40. Fitzpatrick N. Subtotal coronoid ostectomy (SCO) for the treatment of medial coronoid disease: A prospective study of 228 dogs (389 elbows) evaluating short and medium term outcome. In: Congress proceedings of the British Veterinary Orthopaedic Association, Autumn Scientific Meeting- Enigmas of the Canine Elbow, Chester, UK, 2006, pp. 22–29.
41. Danielson KC, Fitzpatrick N, Muir P, Manley PA. Histomorphometry of fragmented medial coronoid process in dogs: a comparison of affected and normal coronoid processes. Vet Surg 2006, 35: 501-512.
42. Tobias T, Miyabayashi T, Olmstead ML. Surgical removal of FCP in the dog: comparative effects of surgical approach and age at time of surgery. J Am Anim Hosp Assoc 1994, 30: 360-362.
43. Bοttcher, P. Accelerated cartilage loss following subtotal coronoid ostectomy. In: Congress proceedings of the American College of Veterinary Surgeons Symposium: Chicago, USA, 2011, pp. 108–109.
44. Preston CA, Schulz KS, Taylor KT, Kass PH, Hagan CE, Stover SM. In vitro experimantal study of the effect of radial shortening and ulnar ostectomy on contact patterns in the elbow joint of dogs. Am J Vet Res 2001, 62: 1548–1556.
45. Holsworth IG. How I manage elbow incongruity. In: Congress proceedings of the 12th European Society of Veterinary Orthopaedics and Traumatology Congress: Munich, Germany, 2004, pp. 78-79.
46. Fox DJ. Radius and ulna. In: Small Animal Veterinary Surgery. Tobias KM, Johnson SA (eds). Elsevier Saunders: St. Louis, MO, USA, 2012, pp. 761–784.
47. Johnston SA. Osteochondritis dissecans of the humeral head. Vet Clin North Am Small Anim Pract 1998, 28: 33-40.
48. Schulz, KS, Fitzpatrick N, Young R. Theory and development of the sliding humeral osteotomy. In: Congress proceedings of the American College of Veterinary Surgeons Symposium, Chicago, USA, 2011, pp. 263–265.
49. Fitzpatrick N, Yeadon R, Smith TJ, Schulz K. Techniques of application and initial clinical experience with sliding humeral osteotomy for treatment of medial compartment disease of the canine elbow. Vet Surg 2009, 38: 261–278.
50. Pfeil I, Torrington A, Vezzoni A. In proceedings: Proximal abducting ulnar osteotomy. KYON Symposium, Zurich, 2014.
51. Acker R, Van Der Meulen GT. Tate elbow preliminary trials. In: Congress proceedings of the 35th Veterinary Orthopedic Society Annual Conference, MT, USA, March 2008 pp. 49-52.
52. Meyer-Lindenberg A, Fehr M, Nolte I. Short and longterm results after surgical treatment of an ununited anconeal process in the dog. Vet Comp Orthop Traumatol 2001, 14: 101–110.
53. Turner BM, Abercromby Rh, Innes J, McKee WM, Ness MG. Dynamic proximal ulnar osteotomy for the treatment of ununited anconeal process in 17 dogs. Vet Comp Orthop Traumatol 1998, 11: 76-80.
54. Krotscheck U, Hulse DA, Bahr A, Jerram RM. Ununited anconeal process: Lag-screw fixation with proximal ulnar osteotomy. Vet Comp Orthop Traumatol 2000, 13: 212-216.




